For many people, the way they style or color their hair becomes an expression of who they are. It can feel a bit like losing part of yourself when more hair than usual ends up in your hairbrush, clumps of hair fall out in your hands, or parts of your scalp become visible. Whether due to poor nutrition, natural changes, or medical disorders, dealing with hair loss and breakage can be a struggle for many women, especially after the age of 50.
Fortunately, we are learning more about the conditions that cause baldness every day. The term alopecia is a blanket term that can refer to several types of baldness, including fur or feather loss in animals. Several types of alopecia can affect humans, with differing causes and treatments. Most types of alopecia that affect people have no physically damaging effects besides the loss of hair. A few types, however, can trigger itching or burning sensations. In this guide, we explore a few types of alopecia and how to deal with them.
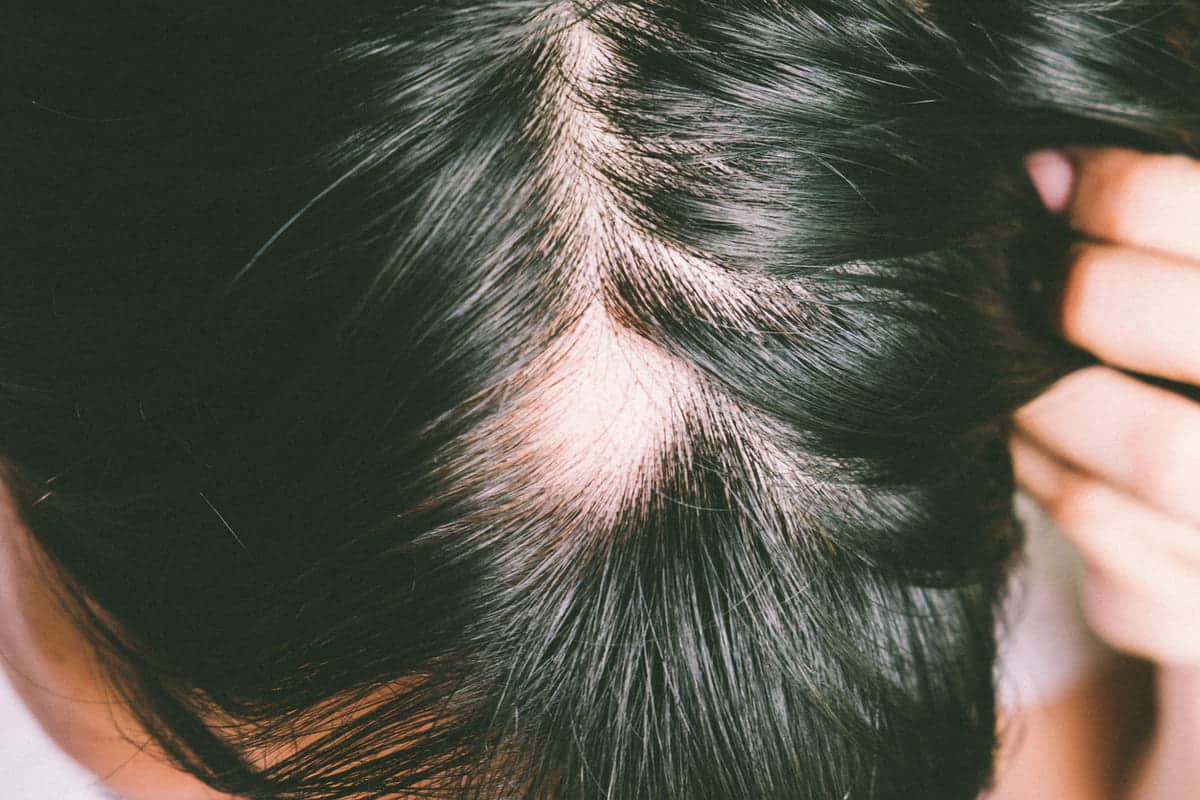
Androgenic alopecia
The most common type of alopecia is androgenic alopecia, a hormone-related loss of hair. It affects approximately 50 million men and 30 million women in the United States alone. Hair thinning due to androgenic alopecia can occur at any point after puberty but is more likely to happen as we reach middle age and beyond.
Changing levels of androgen hormones, particularly the hormone dihydrotestosterone, causes the hair follicles to shrink over time, resulting in a shorter and shorter growth phase. Hair loss due to androgenic alopecia tends to happen in a predictable pattern. This is why it is better known as male or female pattern balding.
Better known as male pattern balding, it usually starts at the hairline when it affects men. It gradually moves backward, often resulting in a U-shaped pattern of hair on the sides of the head as it progresses. Although female pattern baldness has the same triggers as male pattern baldness, it presents as a more uniform thinning of the hair rather than starting at the hairline and moving backward.

Alopecia Areata
Alopecia areata is an autoimmune condition that causes the immune system to target the hair follicles. The stricken hair follicles stop growing hair, leaving irregular bald patches. While we don’t clearly understand what causes autoimmune disorders like alopecia areata to develop, genetics are likely to play a role. Individuals whose relatives have developed either alopecia areata or other autoimmune disorders have a higher risk of developing alopecia areata.
Most people are referring to patchy bald spots on the scalp when they reference alopecia areata, but alopecia areata also includes the following specific forms:
- Alopecia areata incognita—The hair falls out more evenly rather than falling out in patches. Also known as diffuse alopecia areata, it looks similar to female pattern baldness, but the hair loss tends to be more abrupt and intense. It is also more likely to strike younger women.
- Alopecia ophiasis—Hair is lost from the sides and lower back of the scalp, in a band-like formation. Microneedling has been used to treat this particular pattern of alopecia on rare occasions.
- Alopecia totalis—The entire scalp is bald.
- Alopecia Universalis—Bald patches are not restricted to the scalp and can be found all over the body.
Most people with alopecia areata experience their first bald patches before their 30th birthday, and children may also be affected. Children are more likely to experience additional symptoms, including pitting or lesions on the nails.
This condition isn’t as predictable in its progression as pattern baldness, and alopecia areata sometimes even clears up without intervention. In some cases, the spontaneous regression is permanent, while at other times, the patches may reappear.
Circumstances linked to a higher incidence of reoccurrence include:
- Early age at onset
- Extensive hair loss
- Family history
- Multiple autoimmune disorders
- Nail changes
Traction Alopecia

This type of balding is due to the repeated or continuous pulling of the hair follicle. It is usually caused by regularly wearing the hair in tight hairstyles like braids, cornrows, or tight ponytails. If caught early enough, this condition is frequently reversible simply by changing hairstyles.
Cicatricial Alopecia
Cicatricial alopecia is a rarer collection of conditions in which inflammation leads to the destruction of the follicle cells that produce hair. With primary cicatricial alopecias, the inflammation targets the follicles directly. With secondary cicatricial alopecias, the inflammation and damage are preceded by an instigating factor, such as a tumor, an infection, or radiation treatments.
Some individuals with cicatricial alopecia have no major symptoms beyond hair loss, while others may experience itching, scaling, pustules, or changes in pigmentation. It can affect any age or gender, though it rarely strikes children. The damage to the hair follicles is often more intense with cicatricial alopecias, and its triggers are poorly understood. In some cases, the damage to the follicles may become permanent, and scarring may become visible.
Diagnosis
Your doctor may recommend a skin biopsy from the affected area in any of these cases. This helps to ensure that nothing is lurking under the scalp, like an infection. Studying the biopsy will also give them better information about the type, intensity, and extent of the damage to the hair follicles.
Treatments
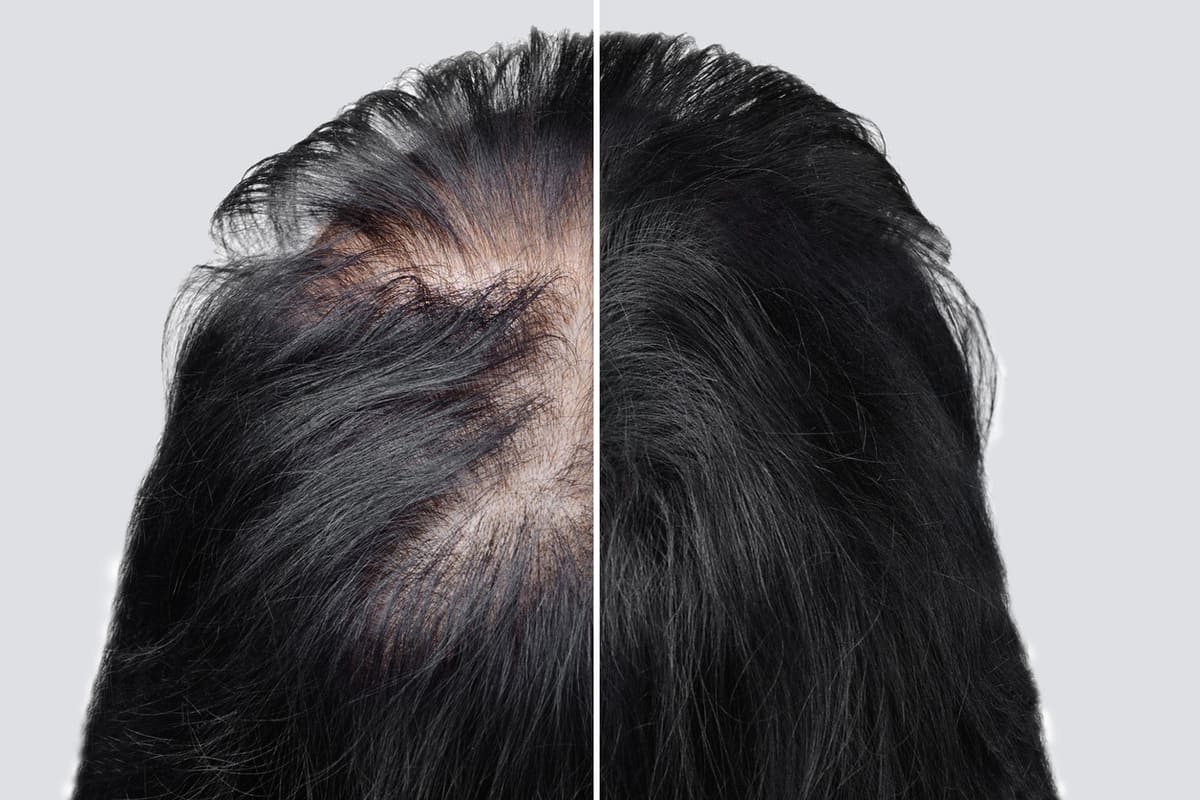
In some cases, especially for those afflicted by a version of alopecia areata, the condition may go into spontaneous remission. In other cases, the hair loss is reversible by using medications or other therapeutic treatments. Sometimes, hair loss isn’t fully preventable. Here are a few of the treatments and medications available for people suffering from alopecia.
Minoxidil
Minoxidil, better known by the trade name Rogaine, is known to stimulate non-functioning hair follicles. It has been approved as a topical regrowth medication for both male and female pattern baldness since 1988. Although it is effective for many people, it may not stimulate growth for all, and it takes months before regrowth is noticeable when it does work. The medication must be reapplied regularly, or the hair loss will reassert itself.
Although it has relatively few side effects, it can cause dry, itchy skin on the scalp. New hair growth sometimes differs in color or texture from the patient’s original hair, and occasionally it can cause hair growth in unwanted areas, such as the cheeks or forehead.
Anti-Androgens
Anti-androgen drugs like spironolactone are especially helpful in reducing the androgens that accelerate hair loss in women.
Hormone Treatment
Hormone replacement therapy alleviates symptoms of androgenic alopecia for some women.
Hair Transplant
Depending on the type and severity of the condition, surgeons move a strip of scalp from the back of the head to fill in an area that has gone bald.
Low-level Light Therapy
Low-level light or laser therapy has been bandied around as a possible solution to alopecia for quite some time—since the early 2000s. A few small trials have shown it to have some promise, particularly when used in conjunction with minoxidil. These findings have not yet been corroborated in larger studies.
Corticosteroids
Corticosteroid injections can be quite effective at encouraging new hair growth in a small area and are often recommended for individuals dealing with alopecia areata. These injections typically need to be repeated several times over a long period of time for the best results. Most treatments take six to twelve months to complete.
Side effects are typically mild. The most common are temporary soreness at the injection site, acne, and skin thinning. In rare cases, corticosteroids can lead to blood sugar imbalances, bone thinning, and a temporary depression of the immune system.
While hair loss can be quite distressing, it doesn’t have to take over your life. There are many different treatment options to help stimulate the growth of hair. If you are experiencing hair loss, contact your doctor to discuss your options.
Read Next:
The Best Haircuts for Thin Fine Hair







