As she turns to look at my father, I study my mother’s profile. I see my grandfather’s nose—the one that bolstered his long-held claim that his mother was Cherokee. As she turns back to me, I see the softly draped skin, mapped with creases that had waited many years to appear. The familiar face is different these days. Her eyes—the same gray-green-blue as mine—are a little clouded. She’s confused.
She has been telling a story about a snowy day, a sled, and my brother and me. It was set in one of the many places we lived as my pilot father moved us around the world. But the air force bases, schools we attended, and towns where we lived are now a jumbled stack of names in her mind. She reaches into the pile and pulls one out. “This was when we lived on base at McChord.” “Hmmm,” I say. “Was it before that, at Chanute? Doesn’t matter—go on. You were saying how cold it was.” She turns to my father. He nods, smiling slightly, then looks down at his clasped hands. She turns back to me, taking up her story. “It was so cold that year. The snow just kept falling.”
She doesn’t want us to know when a fact or name has slipped her grasp. But when you’ve looked into a face for 60 years, you know when those eyes hold fear. You’re aware when the hand that had been smoothing a napkin contracts into a fist; you can see the soft jaw is tightening—with what? Concentration, embarrassment, readiness to fight whatever indignity is next? Maybe all of that, I think, as I realize that my own hand tightly grips a ball of napkin and my jaw aches.
Looking into her eyes, I laugh and nod as she tells how my father came outside to help my brother and me find a better hill when, instead of sailing along, our sled barely skidded forward, then cracked through the icy crust, sinking into the deep snow. I wonder if she’s afraid that we see her sinking—and afraid that maybe we don’t. I wonder how long it will be before I can see that she does not recognize the woman with gray-green-blue eyes who calls her “Mother.”

Many of us are watching people we love disappear from our lives in a different way than we expected. We’re learning that the confusion, sadness, and anger that characterize Alzheimer’s disease aren’t experienced only by the patient. We’re left looking for new ways to interact and trying to find the delicate balance between honoring and respecting our loved ones as adults and doing all we can to ensure their needs are met.
In our case, my 84-year-old father cares for my mother as they remain in their home, 50 miles from family, and without any assistance—even a housekeeper. My father grieves as he watches his bride slowly leave him. He is obviously tired, and we see only intermittent, tiny flashes of his trademark sense of humor. He has his own health challenges, and he doesn’t look well. And yet, he resists all offers of help—thinking, I suppose, that if we don’t make any changes, somehow it’s all less real. This is a cruel disease, perhaps especially so when the family lives in the Never Never Land of unacknowledged need and steadily encroaching disability.
I think I have a better solution, but because I am my stubborn father’s daughter, I know he will change his position only when he is ready. So, I began researching to better understand the disease and to ready myself for the time when he agrees to accept help—or it becomes clear that I absolutely must intervene, regardless of his desire for the two of them to be left alone.
What I’ve learned about loving someone with Alzheimer’s disease
1. Be prepared
Estimates are that half of adults 85 and over have Alzheimer’s disease, so be prepared. Know the warning signs of the disease. Understand the financial situation. Go ahead and have the difficult conversation about your loved one’s wishes and any long-term care insurance, savings, or other resources that might be in place. Find an attorney who specializes in elder law. One appointment, even if you go by yourself, will help clarify what measures might be taken to smooth things if you are facing an Alzheimer’s diagnosis.
2. Seek the advice of a medical professional early
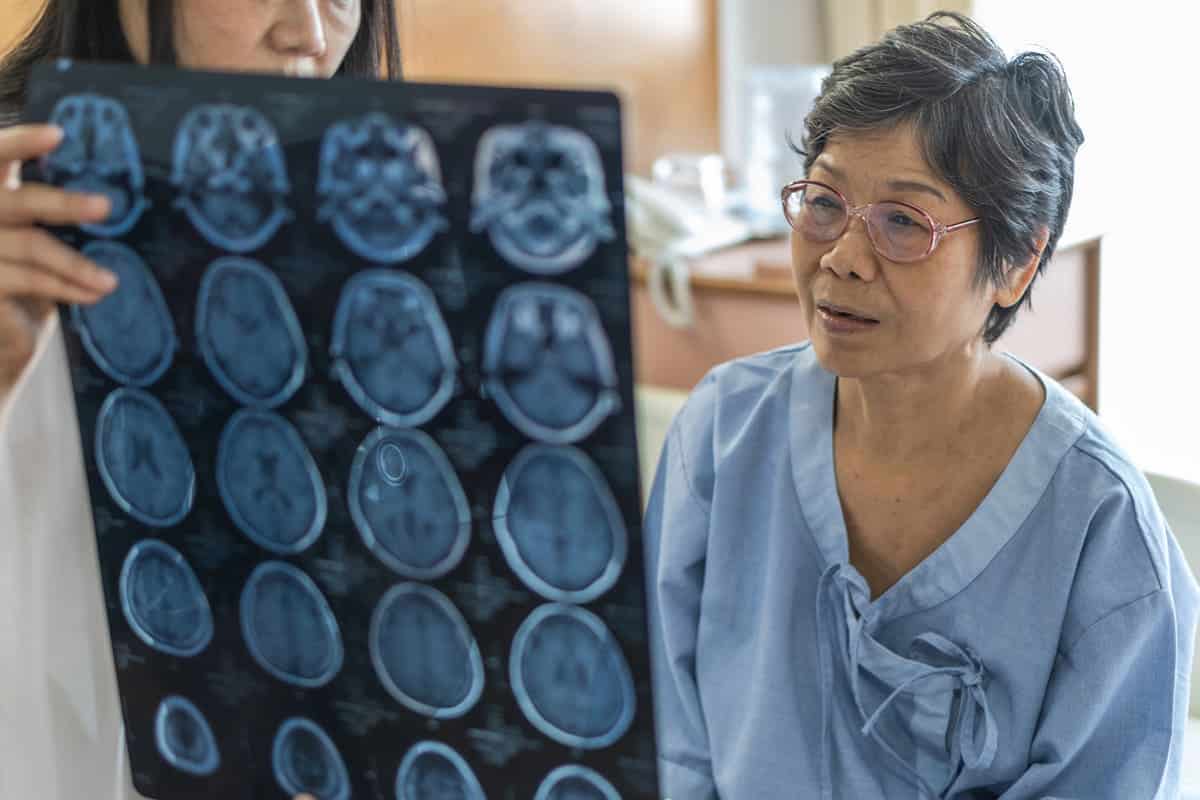
If you begin to suspect there is an issue (don’t second guess yourself—trust what you’re observing), ask your physician for a referral to a medical professional who specializes in diagnosing and treating Alzheimer’s and other dementias. This might be a gerontologist, neurologist, psychologist, or psychiatrist.
Early stage Alzheimer’s, or Mild Cognitive Impairment (MCI), is often difficult to detect – and mild signs of dementia could be caused by something easily addressed, like medication issues or nutritional deficiencies. Even if the diagnosis is Alzheimer’s, having the support and assistance of an experienced medical professional is critically important.
3. Accept help from others
If you are the caregiver, be open to help. There is an increased likelihood of depression, emotional stress, and financial problems among caregivers. Communication difficulties and personality changes that accompany Alzheimer’s cause incredible strain on family members trying to provide care. It can be a lonely and difficult job. Accept help! Many long-term care policies will pay for assistance in the home, from cleaning and cooking to actual nursing care. Even if that’s not an option, don’t say no to the help that is offered. Be as kind to yourself as you want to be to the person you love.
4. Remember the good times
Refresh yourself with photos, videos, letters, or other reminders of your beloved when he or she was graceful, robust, clever, handsome, or beautiful. Remember the stories, the wisdom, and the love you’ve shared. It’s hard to reconcile what you’re seeing with what you remember, but don’t forget to remember! When you’re with them, play music that has particular meaning for them: the soundtrack of their youth, the music they’ve danced to, or sung—or sung to you. Music often stirs a place in the heart that nothing else can reach. If it does, enjoy the trip to sunnier days with them.
5. Educate yourself
Learn the stages of the disease. Learn how to communicate with someone with Alzheimer’s more effectively. Understand the behaviors you can expect to see, and become comfortable with knowing you (and your beloved) have little control over the behaviors—or the occasional heartbreak they cause you. Find resources that are appropriate for you. Even if you’re not the primary caregiver, if this disease is affecting someone you love, it is affecting you. If a sibling or another loved one is the caregiver, you’ll want to know how best to offer support.
Where to find Alzheimer’s disease information and support
- Start with visiting the Alzheimer’s Association website at alz.org. I waited too long to go there (probably thinking, like my father, that acknowledging it makes it real). You’ll find help of all kinds there – information, ideas, and community. Join in a conversation (or just read one) on one of the message boards. People that are dealing with the same issues you face share support, validation, and ideas are there.
- Ask your medical professional about local resources.
- Check with your place of worship to see if they offer a support group or other services, referrals, or support.
- Google “The Best Alzheimer’s Disease Blogs of the Year,” and visit some to see if there are threads that speak to you. Visit sites like “A Place for Mom” even if you’re not looking at care facilities right now. This is not an endorsement of their service, but they do post relevant and helpful articles and links.
Bette Davis said, “Getting old is not for sissies.” Well, neither is loving someone who is getting old—if they are suffering from Alzheimer’s disease. So be kind to yourself, educate yourself and seek and accept support as you share a long goodbye with your beloved.
Read Next:







