Sponsored post.
If you’ve ever noticed hair lying on your pillowcase, wrapped in the bristles of your hairbrush, or swirled around the shower drain, you know how anxiety-provoking this is. We ladies take our hair seriously and never wish for anyone to experience hair loss.
Do you think you could be losing too much hair? If so, you’re not alone. I hear this concern frequently in my practice, with patients often asking if stress and cortisol could be the cause.
After all, in the last two years with the C-19 pandemic, uncertainties in our economy, and now awareness of suffering in Ukraine, there has been a surge of stress, depression, and anxiety. Cortisol rises in times of stress and is a cause of hair loss; however, it is not the most common cause.
The Most Common Cause of Hair Loss

The most common cause of hair loss in both men and women is a deficiency and/or imbalance of Sex Hormones. Stress worsens the balance of sex hormones and escalates their decline but doesn’t cause it. My patients are generally happy to hear this because they want to get to the root of the problem as quickly as possible. Correcting sex hormone-induced hair loss is far simpler than eliminating stress!
As we enter midlife, the levels and balance of 6 Sex Hormones change. A decline in hormones begins about ten years before menopause. Our hair suffers when hormones responsible for hair growth decline or when hormones that promote hair loss are elevated. And it’s ultimately the balance between these 6 hormones that determine the quantity and quality of our hair.
In other words, Hormone Balance is critical. And as a hormone specialist, I can attest that balancing hormones is a true ART that takes decades to master. But before I share more about these 6 hormones, let’s clarify something extremely important that every woman should understand first.
Estrogen Does Not CAUSE Breast Cancer
In 2002, the largest study on women’s hormones, the Women’s Health Initiative, erroneously reported that Estrogen caused breast cancer. Millions of women ditched their hormones, and physicians rarely prescribed them for the next two decades.
After the first decade of re-evaluating the Women’s Health Initiative data, it was revealed that it is not Estrogen that increases the risk of breast cancer. Instead, the synthetic Progestins used in prescription hormone replacement are the culprit. In fact, the group of women who were assigned Estrogen only (without Progestins) had the lowest rates of breast cancer – lower than even the control group who did not use any hormones at all.
What’s really going on.
The American Menopause Society and the American College of Obstetricians and Gynecologists explain Estrogen’s association with breast cancer this way: Estradiol does not cause breast cancer; however, if you have breast cancer, Estradiol may make it grow faster. (You will find out why when we talk about Estrogen Receptor sites below.)
This is the same situation with men and prostate cancer. Men with the lowest testosterone levels are at the highest risk of prostate cancer. However, if a man already has prostate cancer, Testosterone may cause it to grow faster.
We’ve come a long way since the Women’s Health Initiative, and I could not be more pleased. It’s felt that over 100,000 women lost their lives to heart disease between 2002 and 2012 because they were scared to continue their hormone supplementation. And there were millions more who lost their once beautiful thick hair!
Bioidentical Estrogen, at proper, safe, physiologic doses – balanced with bioidentical Progesterone – is critical for our health in every organ of our bodies – especially in our brain, skin, hair, breasts, digestive system, bones, and heart!
6 Sex Hormones that Affect Your Hair
The 6 Sex Hormones that affect hair growth are Estrone (E1), Estradiol (E2), Estriol (E3), Progesterone, Testosterone, and Dihydrotestosterone (DHT). Estradiol (E2), Estriol (E3), and Progesterone promote hair growth, while Estrone (E1), Testosterone, and Dihydrotestosterone promote hair loss.
3 Forms of Estrogen
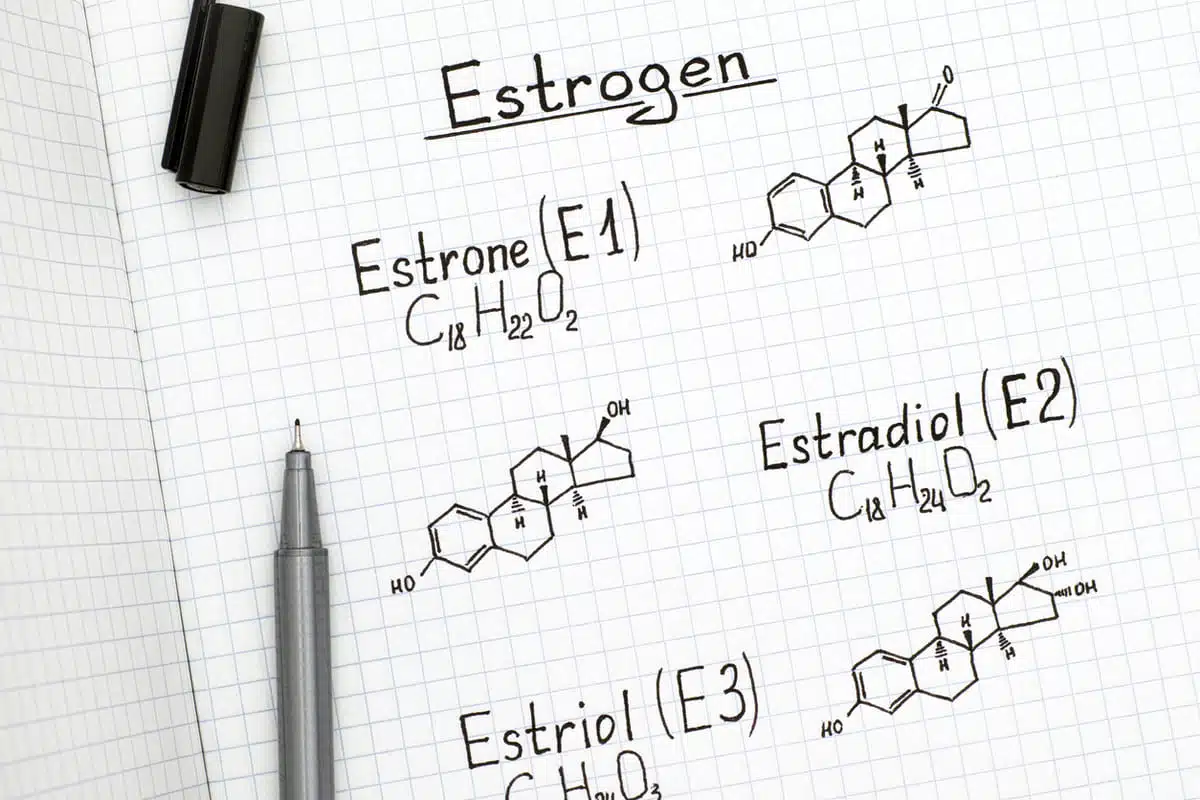
We all have three forms of Estrogen: E1 or Estrone, E2 or Estradiol, and E3 or Estriol. It’s easy to remember which is which by looking at the spelling of each estrogen. E1 has a “one” in Estrone. E2 has a “di” in Estradiol, and E3 has a “tri” in Estriol. Let’s start with the strongest Estrogen and go from there.
1. E2 or Estradiol
Estradiol is the main estrogen our ovaries make during our reproductive years, starting around age 12 or 13 when we begin our menses and lasting through menopause. The cyclical action of Estradiol (E2) during these years is responsible for our monthly period. It is our strongest estrogen and most responsible for maintaining the health and function of all our organs, particularly our heart, brain, digestive system, and bones. It’s also good for our skin, hair, and vagina but not as effective as another form of Estrogen we’ll talk about shortly, Estriol (E3).
Studies have shown that low levels of Estradiol (E2) are associated with higher rates of breast cancer and higher risks of heart disease, bone loss, diabetes, and memory loss. After menopause, we don’t make Estradiol anymore from our ovaries, but we do still have some Estradiol from our body’s conversion of Estrone (E1) – just in very low amounts.
2. E1 or Estrone
Estrone is the main estrogen we make after menopause. But instead of making it in our ovaries, we make it in our fat cells. At one time, it was thought to be stronger than Estradiol (E2) but is now known to be less strong. Initially, it was felt to be stronger because it is more closely associated with breast cancer. Now we know it’s more about the receptor sites Estrone binds to instead of its strength that implicates it more closely to breast cancer.
When it comes to our hair, Estrone (E1) is again the Estrogen we don’t want. Estrone (E1) shortens the growth phase of our hair, pushing it faster into the shedding phase. We want as little Estrone as we can have!
3. E3 or Estriol
Estriol is the jewel of Estrogens. It is also called the “Hormone of Pregnancy” because our bodies make very high amounts of Estriol (E3) during pregnancy. Estriol is associated with lower rates of breast cancer, reduced heart disease, improved bone mass, and is the most effective of all the Estrogens for keeping our vaginas moist and safe from vaginal atrophy.
When it comes to our hair, Estriol (E3) is the strongest Estrogen promoter of hair growth. It does so by directly increasing the growth phase of hair. And since Estriol is very high during pregnancy, our hair grows more quickly during this time. The unfortunate part about our longer, more luscious hair of pregnancy is that Estriol plummets after childbirth resulting in significant hair loss – taking up to a year for our hair to recover.
Estrogen Receptor Sites are the Decision Makers
You may wonder how the three Estrogens can be so different. The answer is in where each of these Estrogens bind to activate their effects inside our cells. These binding sites are called Estrogen Receptors. There are 2 Estrogen receptor sites – Alpha and Beta. It turns out that these receptor sites are the controlling factors in how the different Estrogens act inside our cells.
The Alpha receptor site is associated with higher breast cancer rates and hair loss. Estrone (E1), the Estrogen we want little of, binds mostly to the Estrogen Receptor site Alpha.
The Beta receptor site is associated with lower rates of breast cancer and hair growth. Estriol (E3), the Estrogen we want more of, binds mostly to Estrogen Receptor site Beta. Interestingly, isoflavones that are also known to decrease breast cancer rates also bind to Estrogen Beta sites, just like Estriol (E3).
What about Estradiol (E2)? Interestingly, Estradiol binds equally to both Estrogen Receptor sites Alpha and Beta, acting as a balancer with its very important best friend – Progesterone.
4. Progesterone – Estrogen’s Best Friend
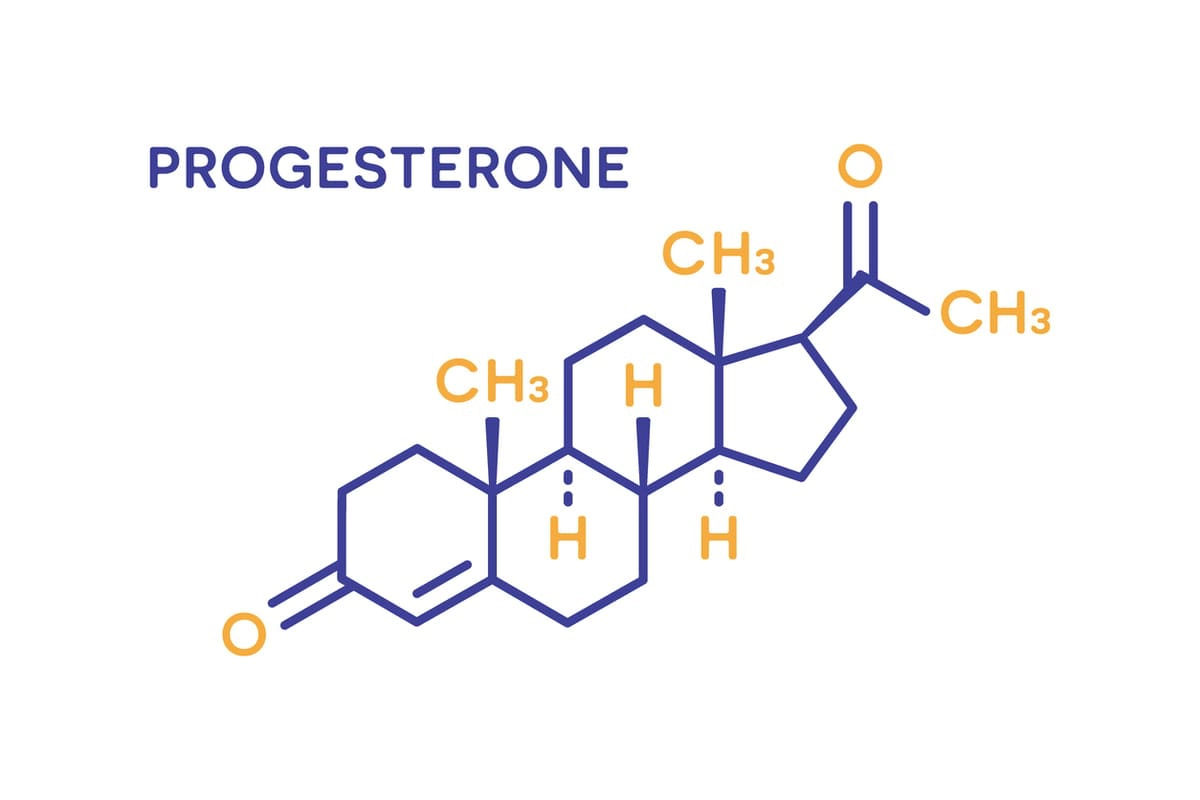
Progesterone is critical in balancing Estrogen’s “growth” effects. Without Progesterone, the growth effects of Estrogen would go unchecked. Unfortunately, Progesterone is the first hormone that declines rapidly 10 to 15 years before menopause. This early decline is the cause of Estrogen dominance, and most women are unaware that this is occurring. The most common symptoms of Estrogen dominance include sleep disturbances, anxiety, breast tenderness, and headaches.
Progesterone also plays a critical and direct role in the prevention of hair loss as well. To clearly understand how Progesterone prevents hair loss, we need to first look at the Hormone Cascade and discover which Sex Hormone is the major cause of hair loss. So, let’s first investigate this and then come back to the beauty of Progesterone.
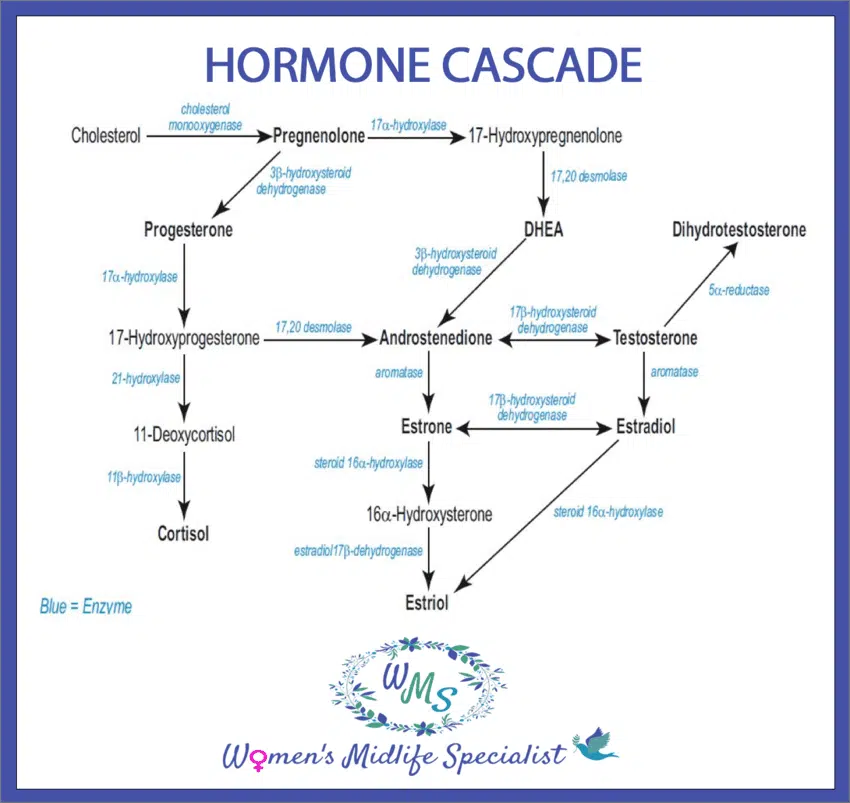
Hormone Cascade: Where Sex Hormones Come From
The Hormone Cascade diagram is shown above and demonstrates how our Sex Hormones are made. All Sex Hormones come from Cholesterol. Pregnenolone is the first hormone that is made from Cholesterol, and from there, it makes either Progesterone or, eventually, DHEA. Most Progesterone goes on to make Cortisol. And DHEA eventually converts to either Testosterone or Estrone (E1).
Following the Hormone Cascade further, you can see that Estrone (E1) converts to the other forms of Estrogen – Estradiol (E2) or Estriol (E3), and DHEA converts to Testosterone. Further still, Testosterone converts to either Dihydrotestosterone (DHT) or Estradiol (E2).
How do these conversions take place?
Enzymes: How Sex Hormones are Converted from One Form to Another
Sex Hormones convert from one hormone to the next by specific Enzymes. The Hormone Cascade diagram shows the names of the Enzymes responsible for each hormone conversion in blue. The two major Enzymes to be most familiar with are Aromatase and 5-alpha reductase.
Aromatase is a very important Enzyme responsible for converting Testosterone to Estradiol (E2).
5-alpha Reductase is equally important to Aromatase because it plays the largest role of all the enzymes in hair loss. It is responsible for converting the Androgen Testosterone to an even stronger Androgen named Dihydrotestosterone (DHT). And it is Dihydrotestosterone which is the real Sex Hormone culprit in causing both male and female pattern baldness.
What about genetics?
Genetics play a role in how active one Enzyme is over another. And in that sense, we have no control. However, we can slow down the action of these Enzymes and balance the conversion of Testosterone to either Estradiol (E2) or Dihydrotestosterone (DHT). And this we do have control over.
By blocking the enzyme 5-alpha Reductase, Testosterone will have higher conversion rates to Estradiol (E2). By blocking the enzyme Aromatase, Testosterone will have a higher conversion to Dihydrotestosterone (DHT). The skill comes with careful blockage of both Enzymes, at just the right amount, to keep our Androgens (Testosterone and Dihydrotestosterone) optimized and balanced with Estrogens.
5. Testosterone: Friend or Foe?
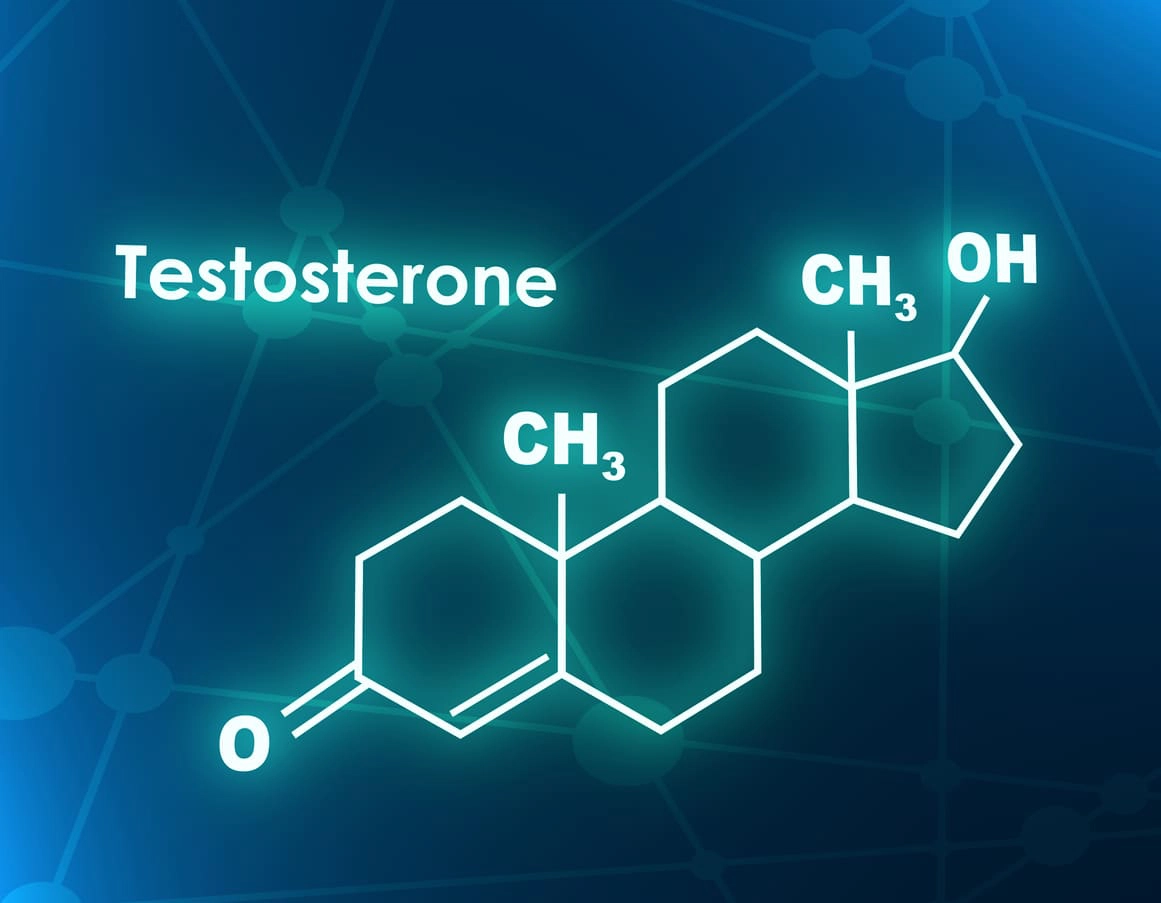
Now that you know Dihydrotestosterone, and not Testosterone, is the Sex Hormone that causes hair loss, you may wonder if you’re better off without Testosterone at all.
Testosterone is a vital hormone we need for energy, confidence, muscle and bone growth, libido, and immune system function. It is also essential for maintaining moisture in our eyes and vagina. So yes, Testosterone is a very important hormone for us ladies! Many research studies have shown supplementation with Testosterone after menopause to be quite beneficial in our quality of life when also well balanced with our Estrogens and Progesterone.
But balance is the key word here. Even women who do not supplement with Testosterone often have an imbalance between their Androgen hormones (Testosterone and Dihydrotestosterone) and hair-promoting Estrogen hormones – Estradiol (E2) and Estriol (E3) – predisposing us yet again to hair loss.
One would think that once our ovaries stop making all the Sex Hormones – Estrogens and Testosterone – we would stop losing hair. Unfortunately, that is not the way it happens.
First, recall that our fat cells make Estrone (E1) after menopause and that Estrone (E1) binds to the Alpha Estrogen Receptor sites, which are associated with hair loss. Next, after our ovaries stop making Testosterone, our Adrenal glands start making it, without being kind enough to also make our hair growth Sex Hormones Estradiol (E2) and Estriol (E3).
This is yet another cause of imbalance between our hair growth Sex Hormones, Estradiol (E2) and Estriol (E3), with our hair loss Sex Hormone, Dihydrotestosterone (DHT), by its conversion from Testosterone. In other words, once our ovaries slow and then eventually stop producing Sex Hormones, Testosterone levels may decline somewhat, but never as much as Estradiol (E2) and Estriol (E3).
6. Fighting the Ravages of Dihydrotestosterone (DHT)
Dihydrotestosterone (DHT) is the single Sex Hormone responsible for male and female pattern baldness. The only way to have Dihydrotestosterone is for it to come from Testosterone. But we need Testosterone, so lowering Testosterone levels is not the answer. So, what can we do?
One method that partially helps reduce hair loss is to supplement with natural 5-alpha Reductase inhibitors. These supplements are sold to reduce the size of the prostate because Dihydrotestosterone (DHT) is also the cause of prostate enlargement in men. My favorite product is manufactured by the brand NOW called Prostate Health. I recommend this product to both men and women to reduce hair loss and reduce Prostate growth in men.
Back to Progesterone’s Beauty
Inhibiting the enzyme 5-alpha Reductase is a partial solution to hair loss; however, it doesn’t address the root cause of hormone imbalances that are taking place as we all move through the seasons of our life. With our newly understood knowledge of the benefits of safe, balanced, youthful hormones, most women should be thinking about hormone replacement.
Recall that Progesterone is an important balancing hormone to our Estrogen and is the first Sex Hormone to decline long before menopause. Progesterone is also a natural 5-alpha Reductase inhibitor. This is how Progesterone is a natural hair growth hormone – by reducing the rate of Testosterone conversion to Dihydrotestosterone. So not only is Progesterone critical to maintaining balance with Estrogen and preventing Estrogen Dominance, but it also helps prevent hair loss by inhibiting the 5-alpha reductase enzyme.
Preferably every woman would have this knowledge early and be prepared for Progesterone replacement 10 to 15 years before menopause, preventing Estrogen dominance. However, even if this opportunity is missed, it’s not too late.
Balancing ALL our Sex Hormones for Hair Growth (and more)!
The absolute most important action we can take to keep our hair growing instead of falling out is to keep our Sex Hormones safely balanced and optimized at natural, youthful levels. Not too much, and not too little. This addresses hair loss at its root cause while also benefiting every organ in our body, including our breasts. You can’t ask for a better solution.
Bioidentical Hormones are identical to the hormones your body makes and can be prescribed by a physician or purchased over the counter. I have been prescribing bioidentical hormones for over twenty years to my patients. However, in 2015, as patients brought their over-the-counter creams to me for approval, I became concerned about the lack of balance and quality of what is available over the counter.
In addition, I am appalled at the lack of education for women so that they can take control of their own health. In 2016, I created the most luxurious line of bioidentical hormone creams, Young Hormones ®, properly balanced at the ratios and amounts that I had been prescribing since 2000. Today Young Hormones® remains the most advanced line of creams, supported by a team of experts to help women of all ages during midlife and beyond.
Congratulations on your new knowledge about Sex Hormones!
You can find our creams here. This link will also help guide you in determining which hormone cream is best for you and help you connect personally with me and my team at the Women’s Midlife Specialist.
Additionally, please enjoy this free booklet, “Do You Think You Might Be Losing Too Much Hair?”
About the Author:

Dr. Karen Leggett (D.O.) is a double board-certified physician, with fellowship training in both Geriatrics and Regenerative Medicine. She is the Founder and CEO of Women’s Midlife Specialist, Inc., Personal Wellness Medicine, LLC, and Leggett Medical Group, Inc. Dr. Karen is also the creator of the Happy Hoo Hoo for vaginal health, and of Young Hormones®, a luxurious line of natural Bioidentical Hormone creams available over the counter.
Dr. Karen is a best-selling author with Brian Tracy in Success Manifesto with Get Energized, Focused, and Downright Sexy Now. She has been a speaker on Hormone Health, Balance, and Optimization to women and medical providers over the past 20 years and has helped thousands of women sail through menopause, reverse aging, and live the life they imagined for themselves as younger women.
You can connect with Dr. Karen at [email protected]. You can also sign up for her free newsletter and discover more about Hormone Health at www.womensmidlifespecialist.com.

References:
(1)Franziska Conrad, Ralf Paus. Estrogens and the hair follicle. Journal of the German Society of Dermatology. May 26, 2004Elise A. Olsen, Female
(2) Pattern Hair Loss, Hair Growth and Disorders, 10.1007/978-3-540-46911-7, (171-186), (2008).
(3) Changmei C, Xiang G, Xiaoxu Y, Xianhui S, Quian D, Qiushi L, Rui X. The roles of estrogen and estrogen receptors in gastrointestinal disease. Oncology Letters 18: 5673-5680, 2019
(4) Maksim Plikus, Elyse Van Spyk, Kim Pham, Mikhail Geyfman, Vivek Kumar, Joseph Takahashi, Bogi Anderson. The circadian clock in skin: implications for adult stem cells, tissue regeneration, cancer, aging, and immunity. J Biol Rhythms. 2015 Jun; 30(3): 1630182
(5) Emily Guo, Rajani Katta. Diet and hair loss: effects of nutrient deficiency and supplement use. Dermatology Practical and Conceptual. www.derm101.com
(6) Sung Choe, Solam Lee, Jaewoong Choi, and Won-Soo Lee. Therapeutic Efficacy of a Combination Therapy of Topical 17 alpha Estradiol and Topical Minoxidil on Female Pattern Hair Loss: A Noncomparative, Retrospective Evaluation. Annals Dermatology. 2018 June: 29(3): 276-282
(7) M. Julie Thornton, Anthony H. Taylor,n Kellie Mulligan,n Farook Al-Azzawi,n Calum C. Lyon,w John O’Driscoll,w, and Andrew G. Messengerz. The Distribution of Estrogen Receptor b Is Distinct to That of Estrogen Receptor alpha and the Androgen Receptor in Human Skin and the Pilosebaceous Unit
(8) Chanda S, Roninette C, Couse J, Smart R: 17beta-estradiol and IC1-182780 regulate the hair follicle cycle in mice through an estrogen receptor-alpha pathway. Am J Physiol Endocrinol Metabolism 278:E202 – E210, 2000
(9) Thornton, J, Taylor, A, Mulligan, K, Lyon C, O’Driscoll, J. Estrogen Receptor alpha and the Androgen Receptor in Human Skin and the Pilosebaceous Unit. Journal of Investigative Dermatology, Volume 8, Issue 1
Andrew M. Kaunitz, MD, reviewing American College of Obstetricians and Gynecologists. New Guidance from ACOG for Treatment of Women with Menopausal Symptoms. Obstet Gynecol 2014 Jan









