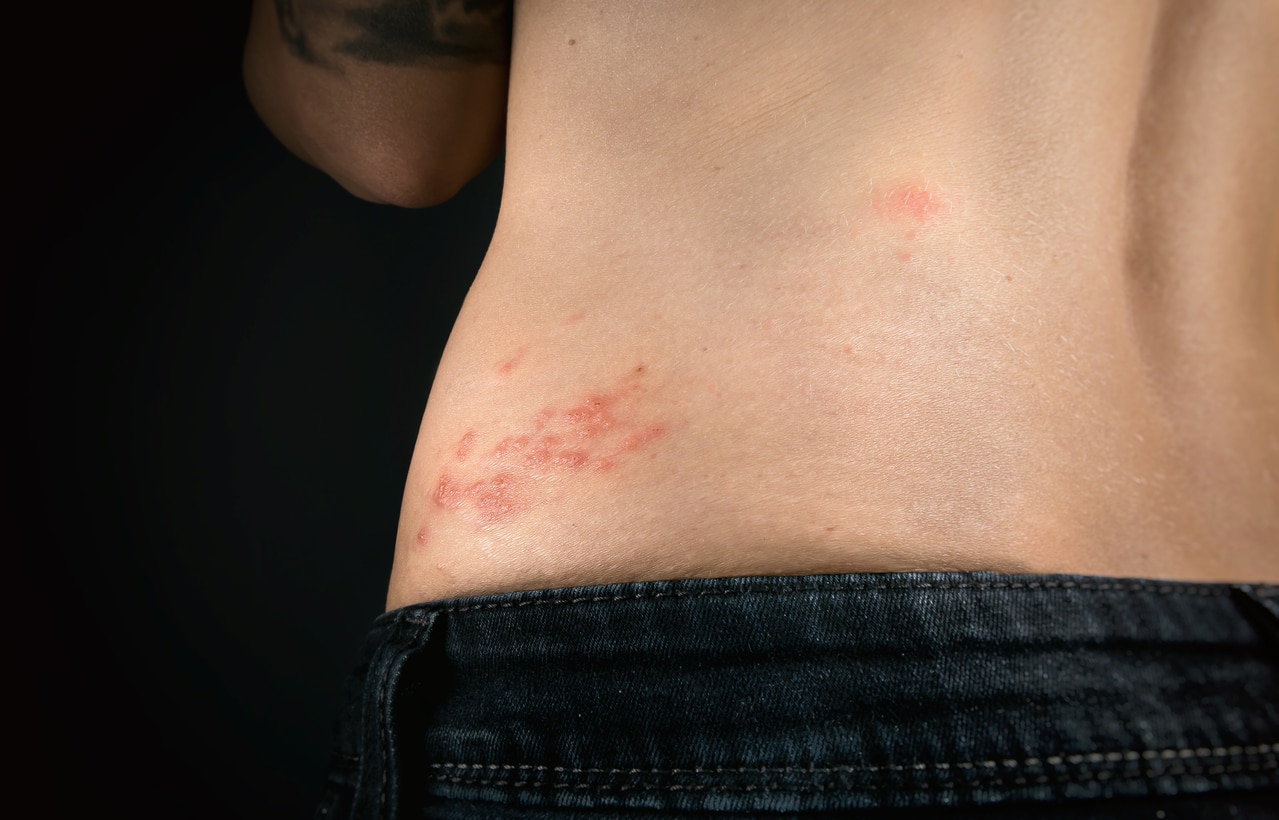
Shingles, also known as herpes zoster, is a viral infection that causes a painful rash. While the word “shingles” may conjure images of roofing materials, the reality is far from benign. This infection is caused by the varicella-zoster virus, the same virus responsible for chickenpox. In this article, we will delve into the intricacies of shingles, exploring its symptoms, causes, risk factors, and available treatments.
Symptoms
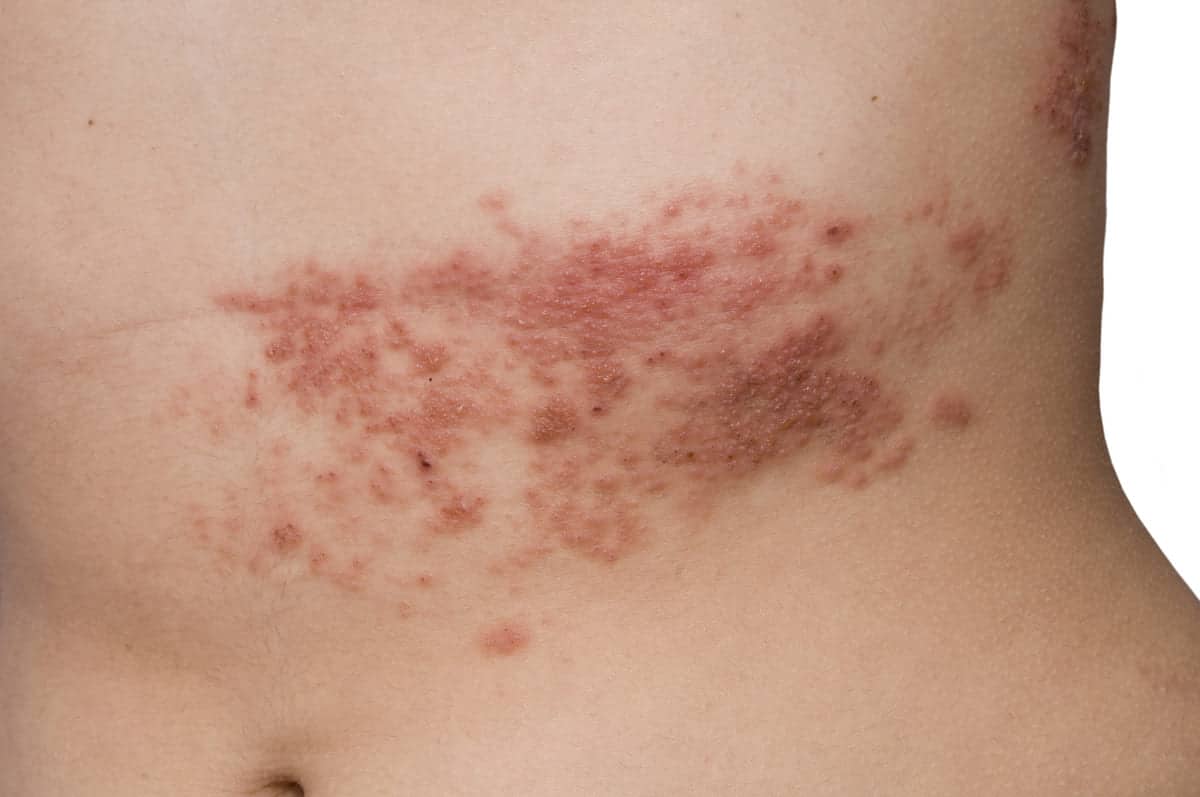
Shingles typically manifests as a painful rash, often accompanied by blisters that can break open and crust over. The rash usually appears in a band, following a specific nerve pathway, most commonly on one side of the torso or face. The pain associated with shingles can range from mild to severe, with some individuals experiencing sharp, stabbing sensations or a persistent burning feeling.
One of the hallmark features of shingles is its association with a condition known as postherpetic neuralgia (PHN). PHN occurs when the nerve pain persists even after the rash has healed, sometimes lasting for weeks, months, or even years. This lingering discomfort can significantly impact an individual’s quality of life, making early detection and treatment crucial.
Causes and Risk Factors
The varicella-zoster virus, which lies dormant in nerve cells after causing chickenpox, can reactivate and lead to shingles. The reasons behind this reactivation are not fully understood, but factors such as a weakened immune system due to age, stress, or certain medical conditions can increase the risk.
Advancing age is a significant risk factor for shingles, with the likelihood of developing the infection increasing markedly after the age of 50. Individuals who have had chickenpox or received the varicella vaccine can still develop shingles, emphasizing the importance of understanding the virus’s ability to lay dormant for years.
Diagnosis and Treatment
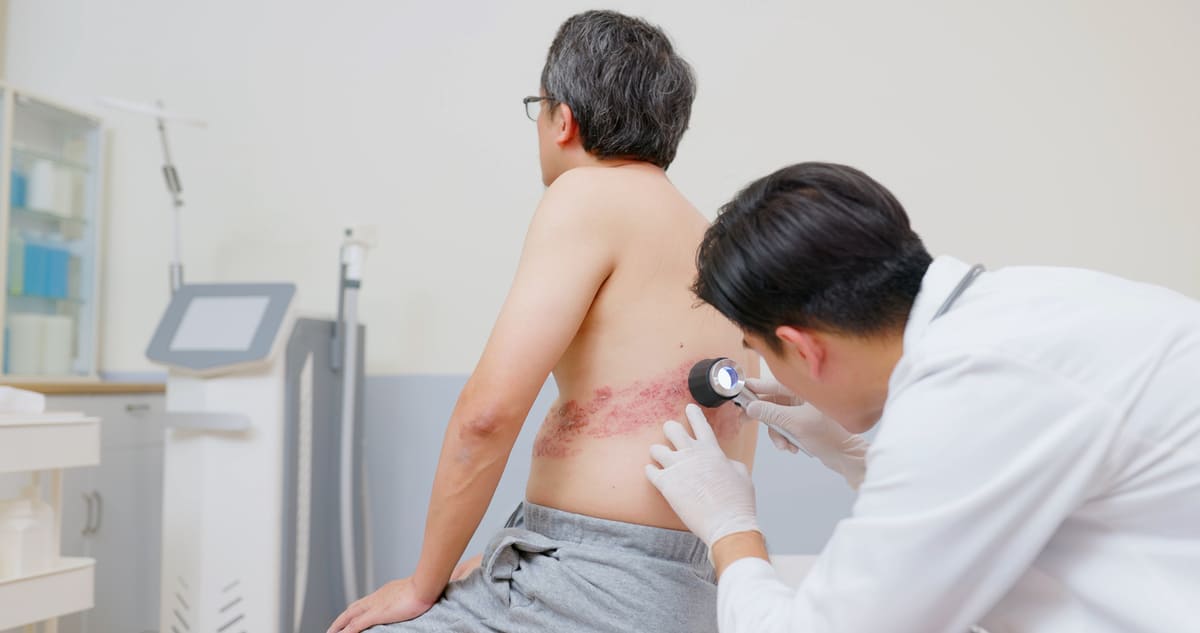
A healthcare professional can typically diagnose shingles based on the characteristic rash and associated symptoms. Laboratory tests may be conducted to confirm the diagnosis or rule out other potential causes of the symptoms.
Antiviral medications, such as acyclovir, valacyclovir, or famciclovir, are often prescribed to reduce the severity and duration of the infection. These medications are most effective when started early in the course of the illness, underscoring the importance of seeking medical attention promptly.
Pain management is a key component of shingles treatment, especially given the potential for postherpetic neuralgia. Over-the-counter pain relievers, prescription medications, and topical creams containing capsaicin or lidocaine may be recommended to alleviate discomfort.
Vaccination
Prevention is a crucial aspect of managing shingles, and vaccination is a key tool in this regard. The shingles vaccine, which is recommended for individuals aged 50 and older, helps reduce the risk of developing the infection and lowers the likelihood of postherpetic neuralgia in those who contract shingles.
There are two shingles vaccines available: Zostavax and Shingrix. Shingrix, in particular, has shown higher efficacy and is the preferred choice for most individuals. The vaccine stimulates the immune system to build protection against the virus. This provides a crucial shield against the reactivation of the varicella-zoster virus.
Conclusion
Shingles is a painful and potentially debilitating condition that can affect anyone who has had chickenpox. While the physical symptoms are challenging, the emotional toll, especially when postherpetic neuralgia sets in, can be equally profound. Understanding the causes, symptoms, and risk factors of shingles is essential for early detection and timely intervention.
The advent of vaccines has significantly improved our ability to prevent shingles and mitigate its impact. As we continue to unravel the mysteries of this viral infection, ongoing research and public awareness efforts play a vital role in minimizing its prevalence and ensuring that individuals at risk are adequately protected. If you suspect you may have shingles or fall within the recommended age range for vaccination, consulting with a healthcare professional is the first step toward effective management and prevention.
Read Next:
The Power of Kojic Acid Soap in Skincare
Are Common Viruses Triggering the Onset of Alzheimer’s Disease?