It can happen anywhere—at a sunny café sipping your favorite drink, on your morning walk, winding down from a long day at work, or enjoying a night out with friends. Out of the blue, you notice tightness or pain in your chest and wonder, could it be a heart attack?
You wouldn’t be irrational for wondering. According to the CDC, 1 in every 5 deaths in the United States stems from heart disease. However, chest pain can be triggered by various conditions and situations, and not all chest pain is the same.
The type of pain, its duration, and its location can provide clues, but cardiac and non-cardiac chest pain symptoms are often extremely similar. In some cases, the symptoms of one so closely mimic the other that only medical tests can prove or rule out cardiac involvement. Here, we explore some of the similarities and differences between cardiac and non-cardiac chest pains.
Cardiac Chest Pain
Cardiac chest pains are those that involve the heart. While heart attacks frequently cause cardiac chest pain, they are not the only condition that triggers heart-related discomfort. Cardiac conditions that can cause chest pain include:
Angina
Angina chest pain is caused by reduced blood flow to the heart. The pain is usually described as squeezing, heavy, or tight and may travel to the neck, jaw, shoulders, or back. This is very similar to the pain experienced during a heart attack, though typically less intense. As with a heart attack, women are more likely to have atypical symptoms, such as nausea, abdominal pain, and shortness of breath.
- Stable Angina– Stable angina is the most common form of angina and can often be managed with medication. Stable angina is more often experienced during exertion, and once diagnosed, it can often be predicted. It is typically short-lived, lasting only five minutes or less, and will resolve more quickly with rest or medication.
- Unstable Angina– Unstable angina is more likely to be a precursor for a heart attack than stable angina. It can occur during either exertion or rest, may last 30 minutes or longer, and neither rest nor medication is as likely to resolve symptoms. *If you or someone you know is experiencing these symptoms, seek medical attention without delay.
- Variant Angina– This is a rarer type of angina triggered by spasms in the arteries of the heart, temporarily reducing blood flow. The pain is often severe and sudden and occurs when resting but may be relieved by medication.
Aortic Dissection
A rare but extremely serious condition, aortic dissection, is when a tear occurs in the inner layer of the aorta. The pain from aortic dissection is usually intense and is often described as a tearing or ripping sensation. There may be a weak pulse on one side or the other, and stroke-like symptoms such as sudden vision problems or difficulty speaking may also be present. *If you or someone you know is experiencing these symptoms, seek medical attention without delay.
Mitral Valve Prolapse
This condition occurs when the valve in the heart fails to close properly. It is usually not a bothersome condition, but it may cause dizziness, palpitations, shortness of breath, and occasional chest pain. Over time, this condition may weaken the heart muscle and should be monitored by a health professional.
Myocardial Infarction
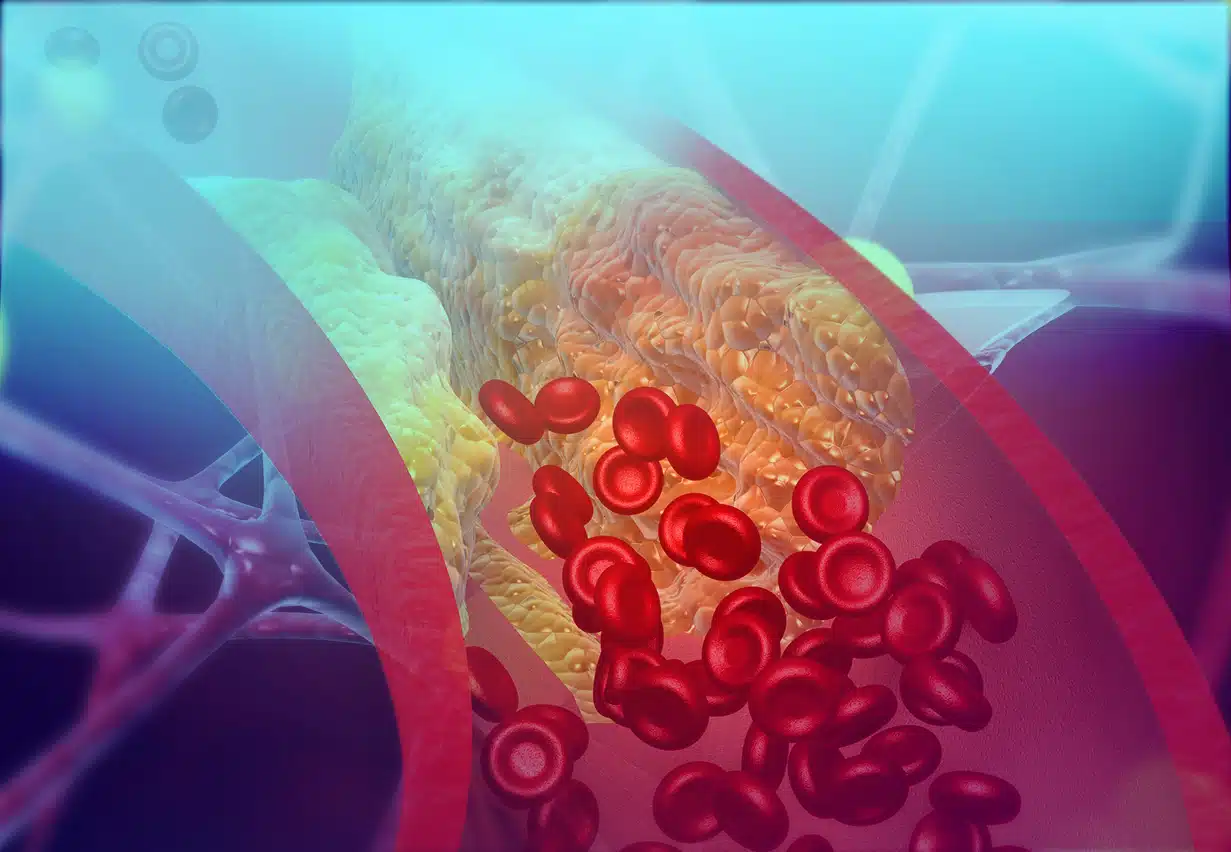
Known more commonly as a heart attack, myocardial infarctions occur when blood flow to the heart is blocked. While women are more likely to experience common symptoms such as cold sweats, sleeplessness, nausea, and severe fatigue, the most prevalent symptom of a heart attack for both men and women is heart pain and pressure in the chest area. The pain of a heart attack often radiates to the arms, upper back, neck, and jaw. It typically lasts longer than a few minutes, although it can sometimes disappear for a short while and then return. *If you or someone you know is experiencing these symptoms, seek medical attention without delay.
Myocarditis
The medical term for inflammation of the heart muscle, or myocardium, is myocarditis. It may be caused by infections, chemical exposure, radiation, and various diseases and conditions. It causes pain and shortness of breath that closely resembles a heart attack and should be evaluated by a medical professional right away. If untreated, myocarditis may result in arrhythmias, blood clots, and permanent damage to the heart muscle.
Pericarditis
Pericarditis is an inflammation of the sac around the heart. Its pain is similar to that of angina or myocardial infarction and should be evaluated by a medical professional. The cause of pericarditis is often unknown. Viral infections, kidney failure, tuberculosis, heart surgery, and certain medications may increase the likelihood of pericarditis developing.
Non-Cardiac Chest Pain
Non-cardiac chest pain is chest pain that is not caused by the heart. There are scores of reasons you might be feeling pain in your chest unrelated to your heart, many of them relatively benign.
Musculoskeletal Chest Pain
Chest pain can be due to injury or insult to the muscles and bones that make up the structure of the chest. Sore muscles, especially around the ribcage, can easily be mistaken for cardiac pain. Muscular pain can be triggered by a number of situations, including working out, strains or tears, chronic pain syndromes such as fibromyalgia, or idiopathic inflammation. Ribs that are bruised or broken can also generate pain similar to cardiac pain, as can conditions such as costochondritis, which affects the cartilage of the rib cage.
Musculoskeletal chest pain typically increases with movement, especially when the chest or upper spine is involved, and may worsen with deep breathing, sneezing, or coughing. When palpitated by the hands, an area of tenderness can sometimes be found that corresponds with the injury. Upper back pain often accompanies musculoskeletal damage.
Digestive Chest Pain
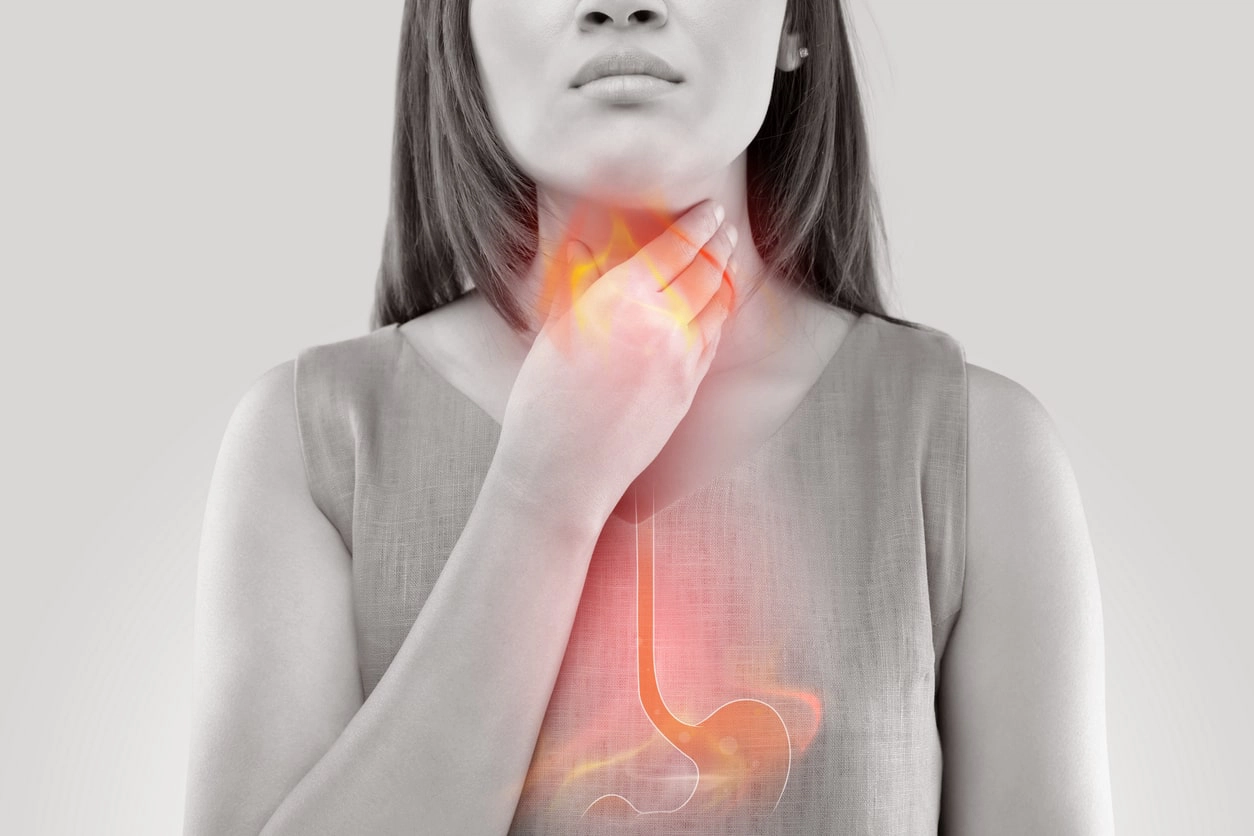
Disorders of the digestive system can frequently lead to pain and discomfort in the chest area. Conditions that affect the esophagus, such as rupture, inflammation, or spasms, can cause pain that is felt in the chest due to a shared nerve system. Inflammation of the gallbladder or pancreas can trigger abdominal pain that radiates from the abdomen to the chest. Pain from stomach problems, such as ulcers and hernias, may also be felt in the chest.
The digestive disorder most commonly mistaken for a heart attack is acid reflux. The pain from acid reflux is felt so close to the heart that it is referred to as heartburn, which can be intense. Pain from acid reflux can often be mitigated with movement or antacids, unlike the pain from a heart attack. Other clues that you may be dealing with acid reflux rather than a heart condition include:
- Bitter or acidic taste at the back of the throat
- Burning rather than squeezing pain
- Pain stays localized to the throat and chest rather than radiating to the shoulders, neck, or arms.
- Pain that increases if you lie down or bend over
- Symptoms are preceded by a large, fatty, or spicy meal
Respiratory Chest Pain
Lung disorders can also cause non-specific chest pain, and like cardiac issues, respiratory chest pain should always be evaluated by a medical professional for a possible cause. While some disorders, like pleurisy, are painful but relatively harmless, others, including pulmonary embolisms, pulmonary hypertension, and collapsed lungs, can become fatal if left untreated. *Those who experience a rapid onset of breathing difficulties and chest pain should seek immediate medical help.
There are many situations and conditions that cause chest pain. Although many of these causes are benign, others can have a dire outcome if ignored. If you are experiencing chest pain, it’s important not to panic and to evaluate the situation. Even if you can rapidly alleviate the symptoms with antacids or movement, be sure to note the time and duration of the pain. This allows you and your doctor to identify any patterns or determine the next steps for further testing. If you cannot relieve your discomfort quickly, it disappears and returns, is accompanied by shortness of breath or nausea, or you are otherwise uncertain, err on the side of caution and call your doctor or health care professional.
Read Next:
Recognize and Prevent Heart Disease







