If you are a woman somewhere around the ages of 40-60, this article is for you. It answers the top 5 questions women ask about hormones and will help you understand what your doctor won’t share or may not even fully understand.
1. Are Hormones Safe?
Hormone therapy is now (and has always been) the number one treatment for menopause and hormone imbalance symptoms because it is the most successful treatment to rid women of the symptoms of menopause as well as prevent chronic diseases such as bone loss, heart disease, dementia, and vaginal atrophy.
The North American Menopause Society (NAMS), recognized as the leading resource on all aspects of menopause for both physicians and the public, released the most recent guidelines on hormone replacement therapy in July 2022. These newest guidelines state that hormones applied topically instead of taken orally (by pill form) are safe for most women and that there is no need to stop hormone replacement therapy just because of advancing age. NAMS guidelines also state that women who have had breast cancer are still candidates for hormones used intravaginally in creams or suppositories.
The following 6 situations require you to have special consideration and should not start hormones without the close guidance of a physician.
- If you have breast cancer
- If you are pregnant
- If you have an estrogen-dependent cancer
- If you have abnormal vaginal bleeding that has not been evaluated by your physician
- If you have a history of clotting problems
- If you have had bad reactions to hormone therapy in your past
2. Will hormones increase my risk of breast cancer?
Over the last 2 decades, recommendations for the use of hormones have made a complete 360-degree circle. This is because, 20 years ago, the largest study of hormone replacement (The Women’s Health Initiative) appeared to reveal that hormones were associated with an increased risk of heart attack, stroke, and breast cancer. This initial data caused worldwide fear in both women and doctors. Many women threw out their hormones, and many doctors stopped prescribing them and set the stage for a turbulent history.
Unfortunately, this data from The Women’s Health Initiative had barely been evaluated when these preliminary conclusions were publicly announced. The media spread these preliminary conclusions haphazardly, resulting in over 50,000 women dying prematurely from heart disease and millions more suffering bone fractures, diabetes, memory loss, and many symptoms of menopause, including hot flashes, insomnia, mood swings, and weight gain.
However, science continued to reassess the data collected from The Women’s Health Initiative over the last 20 years – with the critical facts about hormones now far better understood. Regarding breast cancer, it is now known that:
- Women who take Estrogen have NO increased risk of breast cancer than women who do not take Estrogen. In fact, women who do not use Estrogen after menopause showed a slightly higher rate of breast cancer than those women who DO use Estrogen. We also know that breast cancer risk increases after menopause in women when Estrogen levels are the lowest.
- Women who take synthetic Progesterone (Progestins), which are in synthetic hormone replacements and birth control, DO have a higher risk of breast cancer. Bioidentical Progesterone does not carry the same risk for breast cancer.
Therefore, we now understand it is not the Estrogen specifically in hormone replacement therapy that increases the risk of breast cancer, but the synthetic Progestin that increases the risk.
We also know that the risk of breast cancer is also dependent on other factors, such as how a woman metabolizes Estrogen. Hormones are metabolized by enzymes whose function is dependent on a woman’s individual DNA.
DNA weaknesses called Single Nucleotide Polymorphisms (SNPs) can cause unsafe hormone metabolites to increase inside our cells instead of being cleared safely out of the body. Fortunately, SNPs are modifiable, meaning they can be overcome with lifestyle and nutrition. And today, it is possible to identify a woman’s DNA SNPs and determine what is needed to overcome a woman’s specific DNA weaknesses in metabolizing hormones. This field of medicine is called Epigenetics.
If you are interested in knowing more about your SNPs, I am a certified Epigenetics physician and would be happy to help you discover your personal DNA SNPs.

3. What do hormones do for me?
In addition to the known decline in all-cause mortality (meaning decreased risk of death from all causes), hormones also help prevent heart disease (the number one cause of death), bone loss (the number one cause of fragility), and vaginal atrophy (the number one cause of low libido and painful intercourse).
Hormones also improve many other disease-specific conditions such as insulin resistance, depression and anxiety, fatigue, obesity, arthritis, and gut disturbances like bloating and constipation.
And finally, hormones keep our skin and hair smooth and silky, give us energy, and improve our outlook, passion, and joy for life.
If you are in the mindset of slowing down the aging process, hormones play a large role in the aging process. Between the ages of 35 and 50, your sex hormones decline by 50-75%.
A century ago, this didn’t matter because we transitioned through menopause and then died. But this has changed! Our life expectancy has grown by 30 years in the last century, meaning we can live a vibrant life for 30 or more years past menopause!
4. How can I tell if I need hormones?
As we transition through life, we can often tell that our body is simply running on fewer “cylinders” than it once was. This is often a sign of hormone decline.
Hot flashes are the most common symptom everyone recognizes as a sign of declining hormones, but there are many subtle symptoms too.
Sleep is often disturbed; energy levels are often less than they once were. Hair and skin may feel drier, and interest in sex may decline as well as noticing vaginal dryness or painful intercourse.
Most conventional doctors don’t recommend testing for hormones because they already know levels are declining in our 40s, 50s, and beyond. And there really isn’t a problem with that frame of thinking. But you should have some idea of which hormones you are deficient in and just how severe the deficiency is. I have prepared this Hormone Quiz for you that will help you identify which hormones are declining and how significant the decline has become right now.
Later if you want to home in on assuring balanced hormones and assuring you are using amounts that are keeping you within optimal ranges, testing hormones is also a good idea and can help guide you in tweaking your amounts.
Since topical hormones absorbed through the skin are the safest and most preferred method of hormone use, you need to know the best way to test the tissue levels that accumulate from topical use. This is different than when you use an oral form of hormones – the less desirable form.
To measure levels of oral hormones, regular blood work is appropriate. However, when using topical hormones, the most accurate testing method is a method that will be closest to the lymphatic system because topical hormones travel through the lymphatic system, not as much through the blood. This means either saliva or finger stick blood spot is the most appropriate type of test for topical hormones.
I personally recommend a hormone specialty lab called ZRT Laboratories. ZRT Laboratories are one of the most highly established and respected hormone testing laboratories in the United States, involved in the National Institute of Health and many Universities’ research work.

5. How do I know if I am getting the right kind of hormones?
It’s important to realize that you are in control of your own body and have multiple options when it comes to using hormones.
First, natural, bioidentical hormones are available over the counter. Women’s Midlife Specialist (Young Hormones™) has the most luxurious and varied line of bioidentical hormones available without a prescription that I personally designed as a cosmetic cream with hormone benefits.
Young Hormones are manufactured in the United States in a cGMP, Kosher facility in an all-natural base without any synthetic additives in the exact balanced amounts that I have prescribed to over 95% of my female patients for over 20 years. So, you certainly have excellent options available to you.
You may also want to be aware of what a physician who is not familiar with natural hormones may recommend. Unfortunately, many conventional physicians are still behind the times in their understanding of hormones – either because lack of interest or because most education is guided by pharmaceutical companies. If your doctor is typical, he or she will receive their information directly from the pharmaceutical industry.
In terms of what you can expect, your doctor will likely offer you one of the following choices based on whether you have your uterus.
If you have your uterus, most doctors will likely offer you a combination Estrogen and Progestin. These pharmaceutical hormones come in patch or pill form. You have already learned that the topical (cream/patch) form of hormone replacement is the safest. This is because oral (pill) form increases the risk of blood clots and stroke, so you should always turn any pill form down.
But don’t be fooled by the patch form. Patches have a synthetic form of Progesterone called Progestin and are associated with an increased risk of breast cancer. Names of these Progestins include medroxyprogesterone and norgestimate. All oral contraceptives also have synthetic Progestins, which increase the risk of breast cancer.
On the other hand, if you no longer have your uterus, it is most likely your doctor will tell you that you do not need a Progestin because the Progestin is only for your uterus. But again, this is a detrimental mistake. I suspect this claim was originally created by pharmaceutical companies because all they had to offer was synthetic Progestins since natural Progesterone, which is the only form you should consider, has been available over the counter for decades.
The facts are that many organs in your body need natural Progesterone. In fact, there are over 200 different types of cells in the body that utilize Progesterone. Not synthetic Progestins. So, the initial indoctrination that all doctors received in medical school training was to use an Estrogen with a synthetic Progestin – unless the patient has had her uterus removed. And then, in that case, a woman can forgo the Progestin altogether.
In addition to increasing the risk of breast cancer, Progestins can cause a rise in blood pressure, heart disease, and stroke. They are nothing short of one of the worst “medications” a woman can take. In other words, beware of ALL Progestins.
When it comes to different forms of Estrogen, there are 2 natural forms you can get over the counter and 4 forms of Estrogens you can get from your doctor.
Natural and Bioidentical Estrogens include Estrone (E1), Estradiol (E2), and Estriol (E3). Only Estradiol (E2) and Estriol (E3) are Estrogens we should supplement with and, for that reason, are the only ones you should use. The Estrogen forms in Young Hormones™ (available over the counter) include sole and combinations of Estradiol (E2) and Estriol (E3).
Estrone (E1) is felt to be the form of Estrogen that is associated with Estrogen sensitive cancers. Estradiol (E2) is our reproductive estrogen, and Estriol (E3) is our weakest form of natural estrogen. Both Estradiol (E2) and Estriol (E3) are responsible for the anti-aging effects and health effects of Estrogen.
Estrogens available from a pharmacy include Conjugated Estrogens, Esterified Estrogens, Estradiol-17B, and Estradiol valerate.
Conjugated Estrogens are the most common Estrogen your doctor may prescribe. This is a combination of multiple different types of Estrogens – all from pregnant horse urine – with most of the forms unidentifiable to the human body. Most of the Estrogens in Conjugated Estrogens convert to Estrone (E1), and thus for all these reasons, are not the preferred Estrogen.
Esterified Estrogens are synthetic Estrogens that also are metabolized to primarily Estrone (E1), so again are not the preferred prescribed Estrogen.
Estradiol valerate is a synthetic Estrogen that converts mostly to Estradiol (E2), a more preferred Estrogen, but unfortunately only comes in pill and injectable forms – and thus not the preferred choice.
Estradiol-17B is the last Estrogen available through prescription and is bioidentical, and comes in pill and patch form. Estradiol-17B is the preferred prescribed Estrogen as long as it is in a patch form (not the oral pill form). Remember, if you use the Estradiol-17B patch – make sure you use a bioidentical Progesterone and not a Progestin. So, let’s now turn our attention to your prescription choices of natural, bioidentical Progesterone.
There is only one form of Bioidentical Progesterone available from a pharmacy. And it is not a good choice, which you will see momentarily.
It is called Micronized Progesterone (the name brand is Prometrium). Though this is a fair choice for hormone replacement therapy, it is still not optimal. It is acceptable because both the Estradiol-17B and Micronized Progesterone are both bioidentical, and neither have the negatives of the other pharmaceutical choices that we have already discussed. However, Micronized Progesterone has other undesirable additives, including titanium dioxide, peanut oil, and color additives Yellow No. 10 and Red No. 40. Titanium dioxide is a carcinogen, and peanut oil and color additives are less than desirable.
Here is a chart to summarize the choices your doctor might offer you to help you understand the differences.
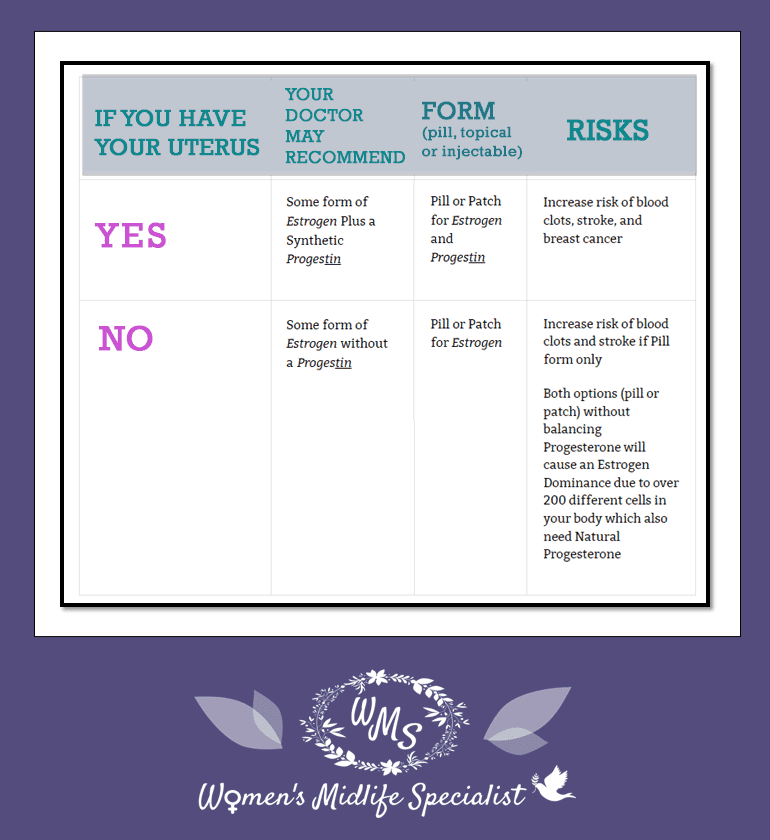
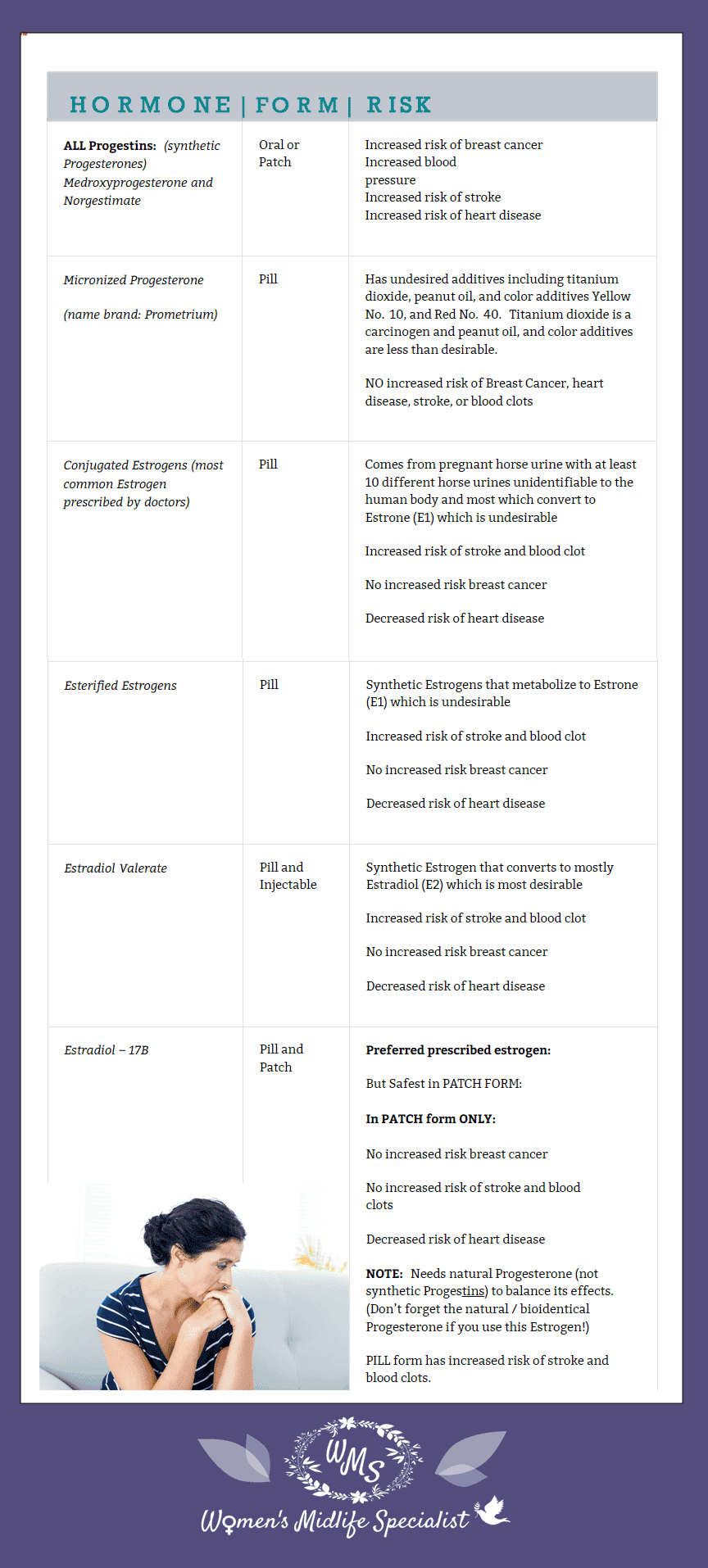
Now that you are chocked full of hormone knowledge, I think you can see exactly why I created Young Hormones™ – because we women need more options to provide us exactly what we want and need.

Now it’s time to take your Hormone Quiz to find out what hormones you may be lacking. (Click the link below.) You will also find a chart outlining your natural options in a special Young Hormones™ chart I have created for you. It defines each beauty and balance cream, as well as when and how to choose and use the right cream for you.
Also, make sure you sign up for our newsletter to continue discovering all you need to know about your beautiful female body, receive special discounts, and connect with me more closely. I look forward to empowering you with more hormone knowledge!
About the Author:

Dr. Karen Leggett (D.O.) is a double board-certified physician with fellowship training in both Geriatrics and Regenerative Medicine. She is the Founder and CEO of Women’s Midlife Specialist, Inc., Personal Wellness Medicine, LLC, and Leggett Medical Group, Inc. Dr. Karen is also the creator of the Happy Hoo Hoo for vaginal health and of Young Hormones®, a luxurious line of natural Bioidentical Hormone creams available over the counter.
Dr. Karen is a best-selling author with Brian Tracy in Success Manifesto with Get Energized, Focused, and Downright Sexy Now. She has been a speaker on Hormone Health, Balance, and Optimization to women and medical providers over the past 20 years and has helped thousands of women sail through menopause, reverse aging, and live the life they imagined for themselves as younger women.
You can connect with Dr. Karen at [email protected]. You can also sign up for her free newsletter and discover more about Hormone Health at www.womensmidlifespecialist.com.
References:
Keep, P.A.; Kellerhals, J. The aging woman. In Ageing and Estrogens. Frontiers of Hormone Research, Proceedings of the 1st International Workshop on Estrogen Therapy, Geneva, Switzerland, 1972; Lauritzen, C., van Keep, P.A., Eds.; S. Karger: Basel, Switzerland, 1973; Volume 2, pp. 160–173. [CrossRef]
https://www.menopause.org/docs/default-source/professional/nams-2022-hormone-therapy-position-statement.pdf; The North American Menopause Position Statement on Hormone Replacement Therapy
Lobo, R.A. Hormone-replacement therapy: Current thinking. Nat. Rev. Endocrinol. 2017, 13, 220–231. [CrossRef] [PubMed]
Stuenkel, C.A.; Gass, M.L.; Manson, J.E.; Lobo, R.A.; Pal, L.; Rebar, R.W.; Hall, J.E. A decade after the
Women’s Health Initiative—The experts do agree. Menopause 2012, 19, 846–847.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6287395/
Grodstein, F.; Stampfer, M.J.; Colditz, G.A.; Willett, W.C.; Manson, J.E.; Joffe, M.; Rosner, B.; Fuchs, C.; Hankinson, S.E.; Hunter, D.J.; et al. Postmenopausal hormone therapy and mortality. N. Engl. J. Med. 1997, 336, 1769–1775.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6780820/pdf/medicina-55-00602.pdf;
The Controversial History of Hormone Replacement Therapy
https://www.news-medical.net/health/Estrogen-Types.aspx: Estrogen Types
https://www.ewg.org/skindeep/ingredients/706561-titanium-dioxide/
https://www.ewg.org/skindeep/ingredients/701829-DC_YELLOW_NO_10_CI_47005/
https://www.ewg.org/skindeep/ingredients/702431-FDC_Red_No_40_CI_16035/
Read Next:
6 Sex Hormones that Affect Your Hair Loss & Growth
The Best Kept Secrets to a Healthy and Happy Vagina










