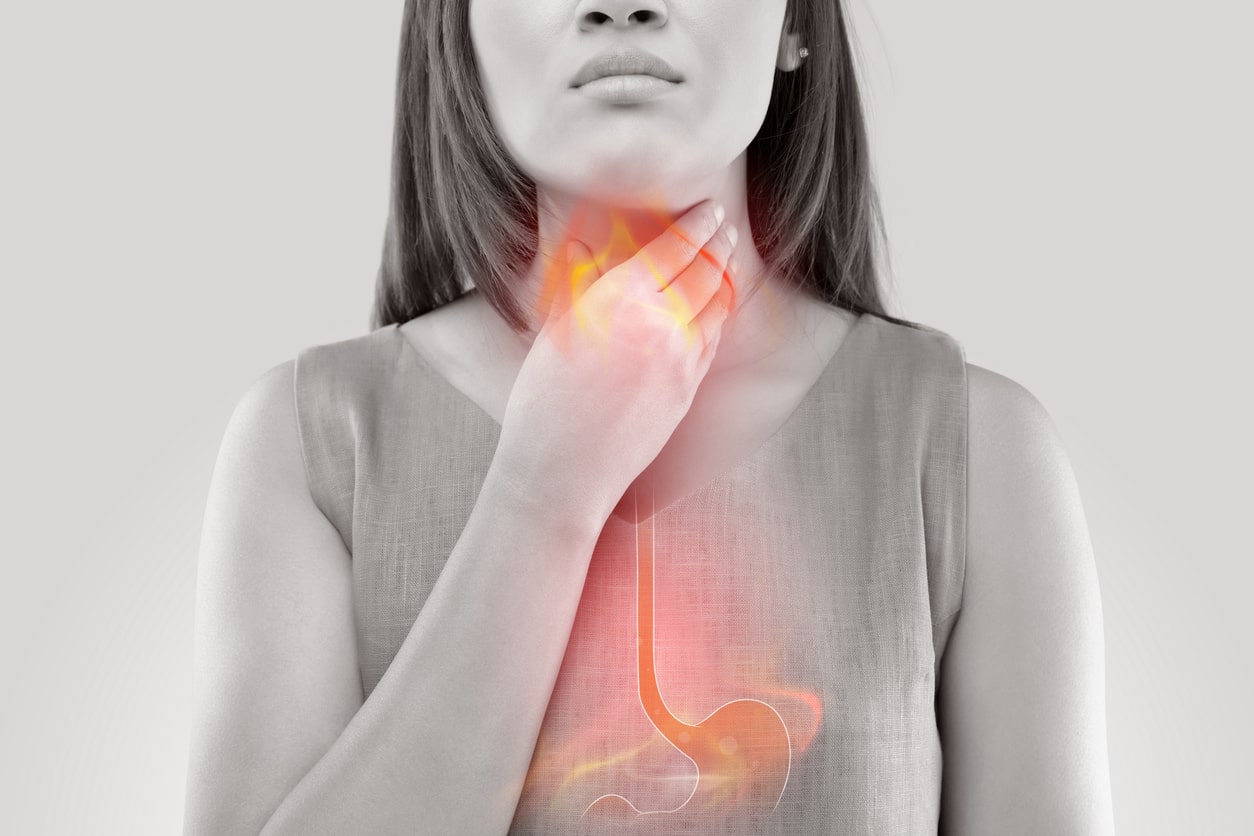
It doesn’t matter if you are sitting in a boardroom, preparing dinner, reading your favorite book, or in the middle of your morning workout—the ball of burning pain that characterizes acid reflux is never convenient. Better known as heartburn, this condition is caused by excess gastric acid traveling up into the esophagus. Unless it becomes chronic, acid reflux can frequently be managed by popping a quick antacid and going on about our day.
Unfortunately, that burning pain also feels an awful lot like the pain of a peptic ulcer. Unlike the occasional bout of acid reflux, peptic ulcers require medical attention. Left untreated, stomach ulcers can lead to dangerous infections and serious blood loss. So how do you know when to worry?
Read on to learn more about the differences between acid reflux and peptic ulcers.
Acid Reflux
The acid in the human stomach can be exceptionally strong, barely less acidic than battery acid itself. The epithelial cells that line the stomach produce a combination of mucus and bicarbonate that coats the inside of the stomach. This mixture provides a barrier between the lining of the stomach and the gastric acids it contains.
Gastroesophageal reflux, more often simply referred to as acid reflux, occurs when stomach acid flows back up the food pipe, irritating the unprotected esophagus. The result is heartburn, which is a burning sensation felt right under the ribs, close to where the heart lies.
GERD, or gastroesophageal reflux disease, is a chronic form of reflux. GERD symptoms include reflux 2 to 3 times a week. The constant irritation may also trigger coughing, regurgitation, and chest pain that is pronounced when lying down.
Too much acid reflux can also cause Barrett’s esophagus.
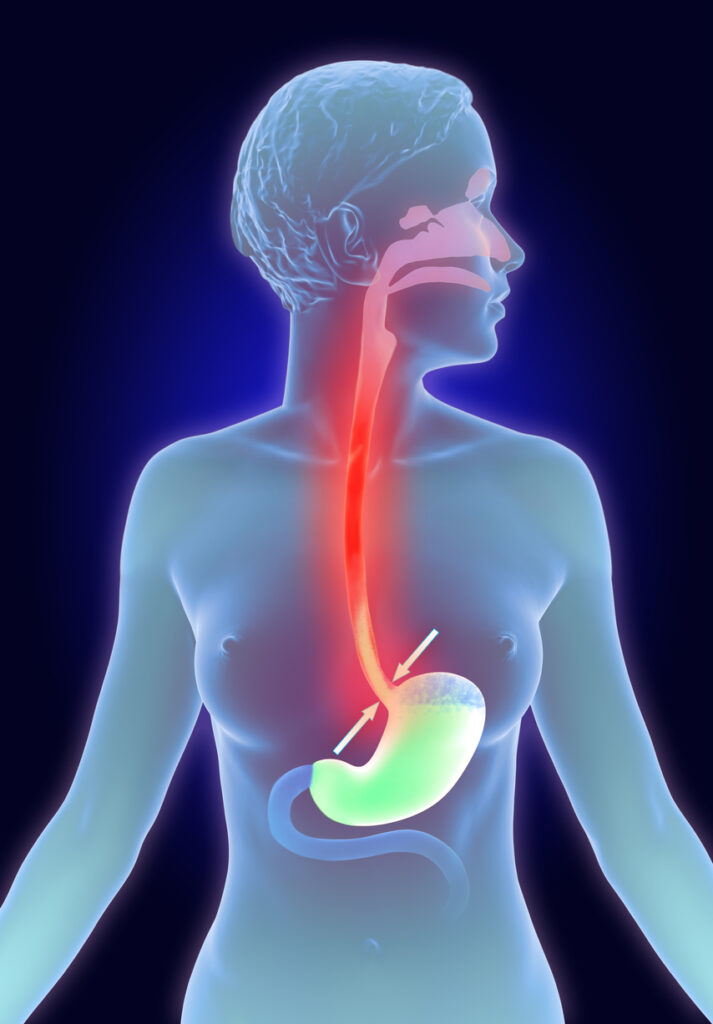
Peptic Ulcers
Ulcers are painful, slow to heal sores that are prone to reoccurring. While ulcers can appear anywhere in the body, some of the most common ulcers are peptic ulcers. Peptic ulcers are formed when gastric juices trigger wounds somewhere in the digestive system. There are three different kinds of peptic ulcers:
Esophageal Ulcers
Ulcers that develop in the esophagus are known as esophageal ulcers. These ulcers are sometimes a result of acid reflux, but not always. Risk factors that may cause esophageal ulcers include taking certain medications, smoking, heavy alcohol consumption, and bacterial, fungal, or viral infections.
The pain from esophageal ulcers is similar to that of acid reflux but may also be accompanied by:
- Bloating
- Dry cough
- Indigestion
- Lack of appetite
- Nausea
- Pain when swallowing
- Sour taste in the mouth
- Vomiting
Gastric Ulcers
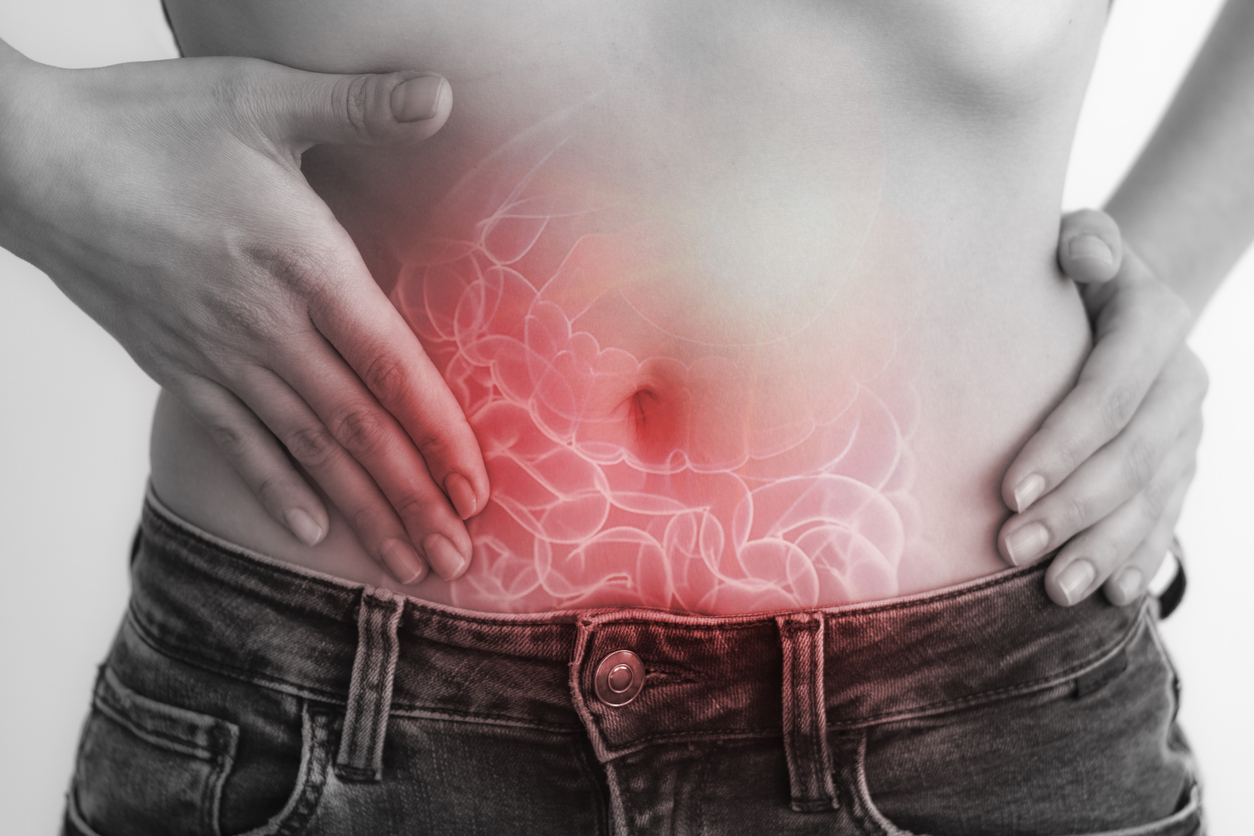
Gastric ulcers develop in the stomach itself. Though frequently characterized by a burning sensation in the stomach area, many gastric ulcers never show any symptoms at all. Symptoms of more severe gastric ulcers can include:
- Appetite changes
- Black or tarry stools (this means you have bloody stool)
- Difficulty breathing
- Feeling faint
- Unexplained weight loss
- Vomiting, including vomiting blood (if it looks like you are throwing up coffee grinds you are throwing up blood)
Duodenal Ulcers
Duodenal ulcers in the upper intestine have symptoms very similar to those of gastric ulcers. Symptomatically, the main difference between these two types of ulcers is when they are triggered. Typically, gastric ulcers are more likely to be triggered shortly after eating, while food is still in the stomach itself. Duodenal ulcers are more likely to strike several hours after eating and may even wake people from their sleep.
The distinction between gastric and duodenal ulcers is just a guideline, however. These types of ulcers should be evaluated by a medical professional to determine their location and severity. A physical examination also helps to rule out or identify dangerous gastrointestinal cancers. Your doctor may choose to evaluate your condition using a series of x-rays known as an upper gastrointestinal series (UGI) or by examining the gastrointestinal tract with an endoscope.
Causes and Prevention for Acid Reflux and Ulcers
Both acid reflux and ulcers are frequently prompted by some of the same triggers and lifestyle choices. Physical issues such as obesity, pregnancy, and heredity components can play a role in either condition. Lifestyle choices such as smoking tobacco, frequently indulging in large or rich meals, consuming acidic foods, drinking coffee, or taking certain medications such as NSAIDs, SSRIs, and steroids can also aggravate either condition.
In addition, acid reflux can be caused by:
- Connective tissue disorders
- Hiatal hernias
- Weakened esophageal sphincter
While ulcers may also form due to:
- Helicobacter pylori infection (also referred to sometimes as h. pylori infection)
- Caustic injury due to ingestion of corrosive substances
- Stress
- Low fiber diet
- Zollinger-Ellison syndrome
- Hypercalcemia
Acid Reflux and GERD Treatments
An occasional bout of acid reflux is more annoying than dangerous. Still, repeated episodes can lead to the narrowing of the esophagus, increased risk of esophageal cancer, and, of course, esophageal ulcers. Infrequent acid reflux is easily managed with over-the-counter antacids, but overuse of these medications can eventually become damaging. Symptoms of calcium overdose due to overuse of antacids can include nausea, vomiting, and the formation of kidney stones.
For those with GERD, alternatives to calcium-based antacids may be suggested. H2 receptor blockers such as Pepcid and Tagamet are one option your doctor may recommend. These inhibit the production of gastric acid at a cellular level. Proton pump inhibitors reduce acid in the stomach by blocking the enzyme that creates gastric acid. Medications like Prilosec, Nexium, and Prevacid are in this class of drugs.
In rare cases, surgery to strengthen the lower esophageal sphincter is required to correct the symptoms of GERD.
Treatment for Ulcers
Antibiotics that are effective at killing the H. pylori bacteria are frequently prescribed to help eradicate any infections. Medications such as H2 receptor blockers or PPIs that reduce gastric acid are often recommended for peptic ulcers. This helps give them time to heal from the initial damage. Formulas like Pepto Bismol that coat the inside of the stomach may also provide a layer of protection for the stomach lining.
Patients will need to refrain from NSAID painkillers, alcohol, tobacco smoke, and acidic foods during their treatment and recovery periods.
Severe ulcers or ulcers that do not respond to treatment may require surgery. Depending on the location and severity of the ulcer, surgery could take several forms, such as:
- Cutting the nerve that controls the production of gastric acid
- Patching the ulcer
- Removal of the ulcer
- Tying off bleeding vessels
Treatments for acid reflux, GERD, and even peptic ulcers are typically effective, and surgery is much rarer than it used to be. Acid reflux is often a chronic issue, however, and ulcers frequently reoccur. In most cases, lifestyle changes, such as eliminating smoking, exercising more, or simply avoiding certain foods, will be needed to experience lasting change when it comes to either condition.
Read Next: