So the fact that your body at 40 or 50 is a bit different from your body at 25 probably comes as a surprise to exactly nobody. Menopause happens to us all.
As bodies change with age, the way we behave in them needs to change as well. So what do your docs – and in particular your ob/gyn – want you to know and do now that you’re 40 or more?
Board-certified ob/gyn, NAMS-certified menopause practitioner, owner of RENUvaGYN, and genneve Director of Health Dr. Rebecca Dunsmoor-Su filled me in on all the details for the Care and Feeding of Your Over-40 Body.
The Big 3 Screens: Breast, Cervix, Colon
Once you reach middle age, your risk of certain kinds of cancer increases. So it’s important to get regular screenings, says Dr. Rebecca. However, what constitutes “regular” differs according to your risk factors. If you’re healthy and have no family history of any of these cancers, you can screen less frequently.
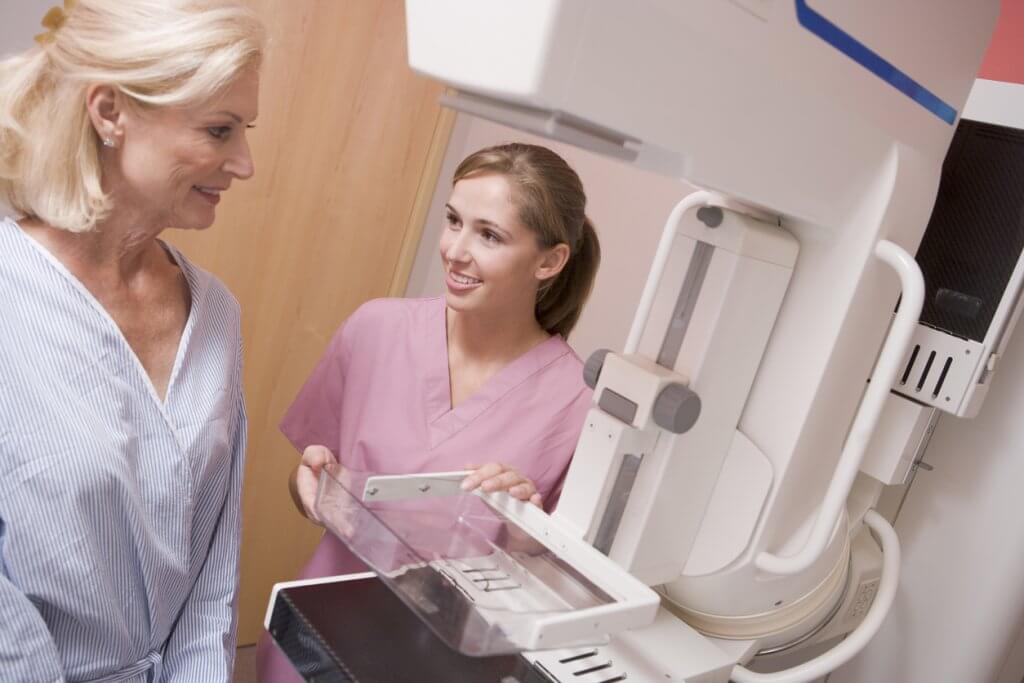 Breast: Mammograms every year or two through your 40s
Breast: Mammograms every year or two through your 40s
Colon: Screenings now start at age 45, which is younger than previously recommended. You should have a colonoscopy every 10 years up through age 75. There are other, stool-based tests that you can opt for, though they need to be done more regularly: the FIT and gFOBT are annual; a stool DNA test (MT-sDNA) is every 3 years.
Cervix: Pap smear done every 1 to 5 years. Talk with your doc about your HPV status and other risk factors to determine the right interval. Even if you’re menopausal, you still need this exam.
STDs
In fact, thanks to the prevalence of erectile dysfunction meds (and other factors), the rate of STD infections is on the rise among Americans 45 or older.
Menopause does not protect against STDs; in fact, the thinning of vaginal tissue caused by a decrease in estrogen can actually make it easier to be infected as the tissue can more easily tear or abrade during intercourse. As long as you’re having sex, says Dr. Rebecca, you should be using condoms.
Pregnancy Risk
Even if your periods are wonky, as long as you’re still having them, you can still get pregnant. Menopause is officially defined as a full calendar year since your last period, so until you pass your “meno-versary,” you should be using contraception.
Eating and Fitness
“This is a great time to address eating and fitness habits,” Dr. Rebecca says, “because as you head into menopause, weight tends to rise a bit, naturally and fitness becomes harder to achieve.” During our busy 20s and 30s, you could get away with more, but now it’s time to focus on you and your health.
Walk half an hour or 45 minutes a day. The rule that’s “out there” is 10 minutes a day minimum, but Dr. Rebecca recommends at least 30 minutes. “A 30-minute walk can be incredibly relaxing as well as good exercise,” she says. “It’s a chance to clear your head and reduce your stress, so take advantage of all the benefits.”
As far as diet, now is the time to capitalize on the good habits you already have and slowly erode the bad ones. Some things to bear in mind:
- Focus on whole foods and grains and steer clear of processed foods. The less processing your food has endured, the better.
- Regarding supplements, it’s best if you get your nutrition from the foods you eat, so you don’t need to supplement. Be sure your diet is sufficiently varied with lots of nourishing veggies.
- However, vitamin D and calcium are super important to keep bone mass from declining. You can’t build new bone now, but you want to keep the mass you’ve got, so Dr. Rebecca recommends supplementing these two critical nutrients. Take them together to maximize their effects.
Cholesterol, Diabetes, Thyroid, and Blood Count
Most of us understand the need to check cholesterol levels, especially if we have a personal or family history of heart disease, but a blood count can also be a useful tool for other health concerns.
Women in midlife and menopause may be at higher risk of developing diabetes, so if you have risk factors, you can include this screen in your blood work as well. If you are 45 or older and have no other risk factors or family history of diabetes, you should be screened every three years, says the American Diabetes Association.
Additionally, you should probably have your thyroid function screened every year or two, says Dr. Rebecca; again, family or personal history of thyroid disease may change the recommended frequency.
With the blood count, the doc is looking to see if you may be anemic. Some medications can reduce your absorption of iron, so it’s good to keep an eye on this. Your doc may also look at the blood work to check that you’re getting enough nutrients.
Heart Disease
 Unless you have a specific concern, Dr. Rebecca says you probably don’t need what’s called a “stress test” or “stress EKG” where they wire you up and put you on a treadmill to check how your heart is working. Generally this test is reserved for people who already have symptoms or history of heart disease or other risk factors such as diabetes.
Unless you have a specific concern, Dr. Rebecca says you probably don’t need what’s called a “stress test” or “stress EKG” where they wire you up and put you on a treadmill to check how your heart is working. Generally this test is reserved for people who already have symptoms or history of heart disease or other risk factors such as diabetes.
What she does want you to know is that heart attacks can look very different in women and men. Women may have jaw pain, shoulder pain, nausea, excessive sweating; the crushing pain under the sternum that we classically associate with heart attack is more common in men and may not be present in women.
Also, many of us still regard heart issues as primarily affecting men. Not true: about 10 years after menopause a woman’s risk is equal that of a man’s. Heart disease is the #1 killer of all genders, so it’s important to pay attention to your heart.
OB/GYN Stuff
Incontinence: If you’re having any leaking, Kegels, Kegels, Kegels, says Dr. Rebecca. Make them an everyday part of your exercise regimen, because continence issues don’t solve themselves. In fact, don’t wait until you have a problem; any woman can and should be doing pelvic exercises to strengthen the pelvic floor. Bonus: better orgasms. However, you might want to get some guidance on how to do the exercises properly, since a too-engaged pelvic floor can also be problematic. Check out a pelvic physical therapist for great, expert advice.
Vaginal tissues: Please talk with your doc. Don’t self-diagnose, don’t self-medicate, don’t clean it with products, and really truly consult with an ob/gyn if you have concerns or questions about any product that’s advertised (or rumored) for use intra-vaginally. Just because someone’s a celebrity doesn’t mean they’re fully informed on vaginal atrophy or pelvic health.
Infections: If you’re getting frequent infections, check with your doctor. Frequent UTIs can indicate menopause; frequent yeast infections can be an early warning sign of type-2 diabetes.
Sex: Use lubes. Always, every time, says Dr. Rebecca. Make it part of the fun. Lubes can protect the tissue from the friction and reduce the risk of infection.
How to Talk With Your Doc
Finally, Dr. Rebecca urges all women to be very direct with their doctors.
Many women feel unheard or dismissed by docs, she acknowledges, so it’s important to be as clear and upfront as you can. Let the doctor know what you’re experiencing, but if you have a specific concern, let him or her know that too. The doc may be able to explain why they don’t share that concern, or she may follow you on that path to see if it’s a factor.
Be direct, and if you don’t feel heard, you’re perfectly within your rights to find a doctor who you trust. However, Dr. Rebecca adds, just because the doctor isn’t saying what you want to hear doesn’t mean she isn’t listening.
Aging and menopause are your body’s way of saying “Take care of YOU.” You’ve likely spent a good chunk of your life caring for kids, taking care of your career, your home, friends, family, etc. and that’s great. But to age well may mean diverting some of your attention back to you, to habits and behaviors that not only keep you healthy but also give you joy.
Read Next:
OB-GYN Shortage: How Tech is Filling the Care Gap for Menopause Treatment
A Bonafide Answer to Menopause Relief







