Our hands and feet are more susceptible to temperature changes than the rest of the body. The smaller size of the blood vessels in the hands and feet increases the chance that cold-related vasoconstriction—the narrowing of the blood vessels—will impede blood flow to these areas. Not only can this lead to discomfort in extreme cases, but it may also lead to frostbite. Additionally, the feet have more nerve endings per square centimeter than most parts of the body, making the cold more noticeable.
Although cold feet can be caused by a cold climate or inadequate heating, these aren’t the only factors. Indications that your cold feet may warrant a visit to your doctor include:
- A change in color (pale, red, blue, or purple)
- Associated cramping in the feet or lower legs
- Leg weakness
- Longer than average rewarming time
- Pins and needles sensations
- Poorly healing wounds
- Swelling or numbness in the feet
- Throbbing pain
11 Conditions that Cause Cold Feet

Certain conditions can make it much more likely for someone’s feet to become cold. Conditions that affect the circulation in the feet make it harder to recover from cold temperatures and may increase the individual’s chances of frostbite or infection.
Anemia
People who have too little hemoglobin in their blood are categorized as anemic. Anemia causes poor circulation, leading to less blood being delivered to the extremities and resulting in cold hands and feet.
Blood Clots
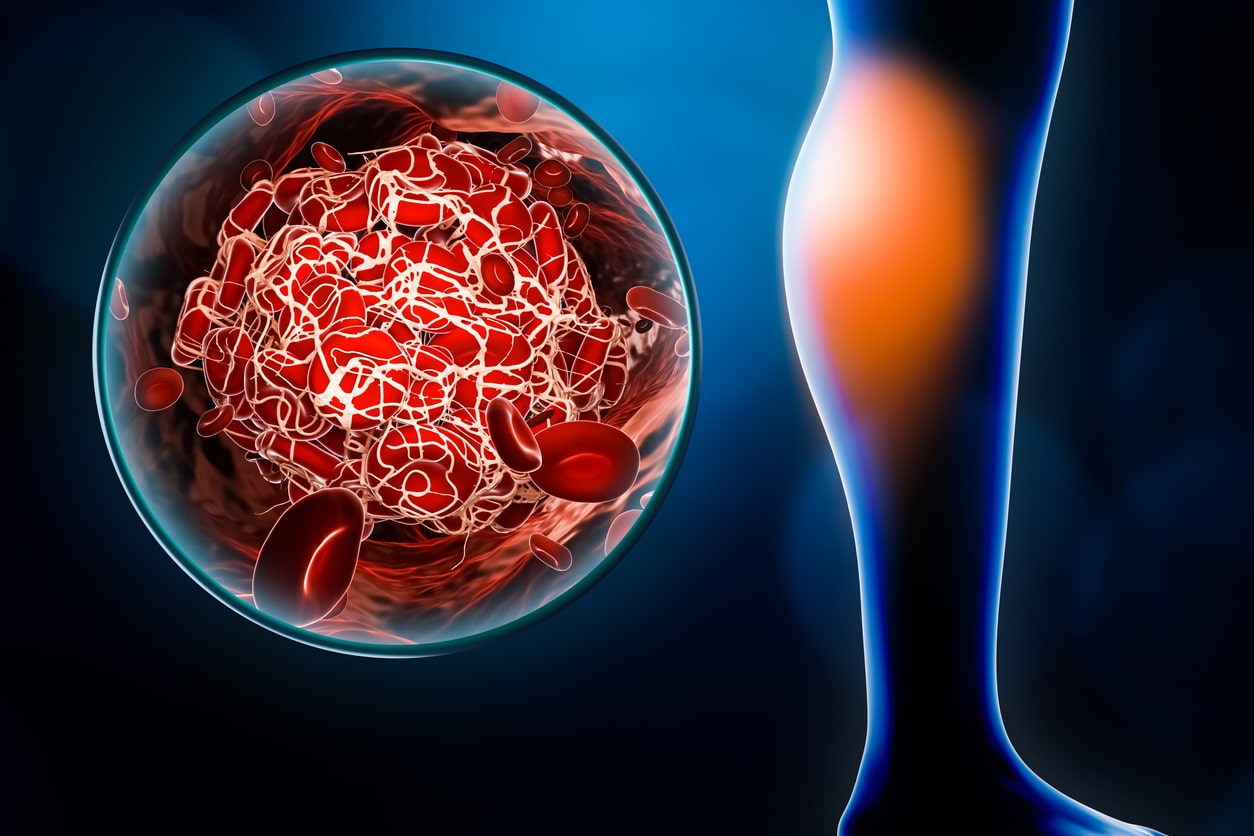
Blood clots that block the flow of blood to the feet may result in cold feet, pins and needles, or even fully numb feet. In some cases, blood flow will be blocked from one foot but not the other, leading to only one foot feeling cold. If you suspect a blood clot, it should be treated as a medical emergency. Contact a medical professional immediately.
Diabetes
High blood sugar levels can cause damage to the nerves, including the nerves in the feet. This may result in burning sensations, feet that feel cold, and in some cases, a lack of feeling in the feet altogether.
Heart Disease
Heart disease weakens the heart, reducing the effectiveness of the circulatory system. This frequently leads to chronically cold hands and feet.
Hormone Fluctuations
Hormone fluctuations, particularly fluctuations in estrogen, testosterone, and thyroid hormones, can constrict the blood vessels. Cold feet frequently develop during menopause due to hormonal fluctuations.
Nerve Conditions
Nerve conditions, such as peripheral neuropathy, may also cause a person’s feet to feel cold or numb. Feet that feel cold but aren’t cold to the touch may suggest a nerve disorder.
Peripheral Artery Disease
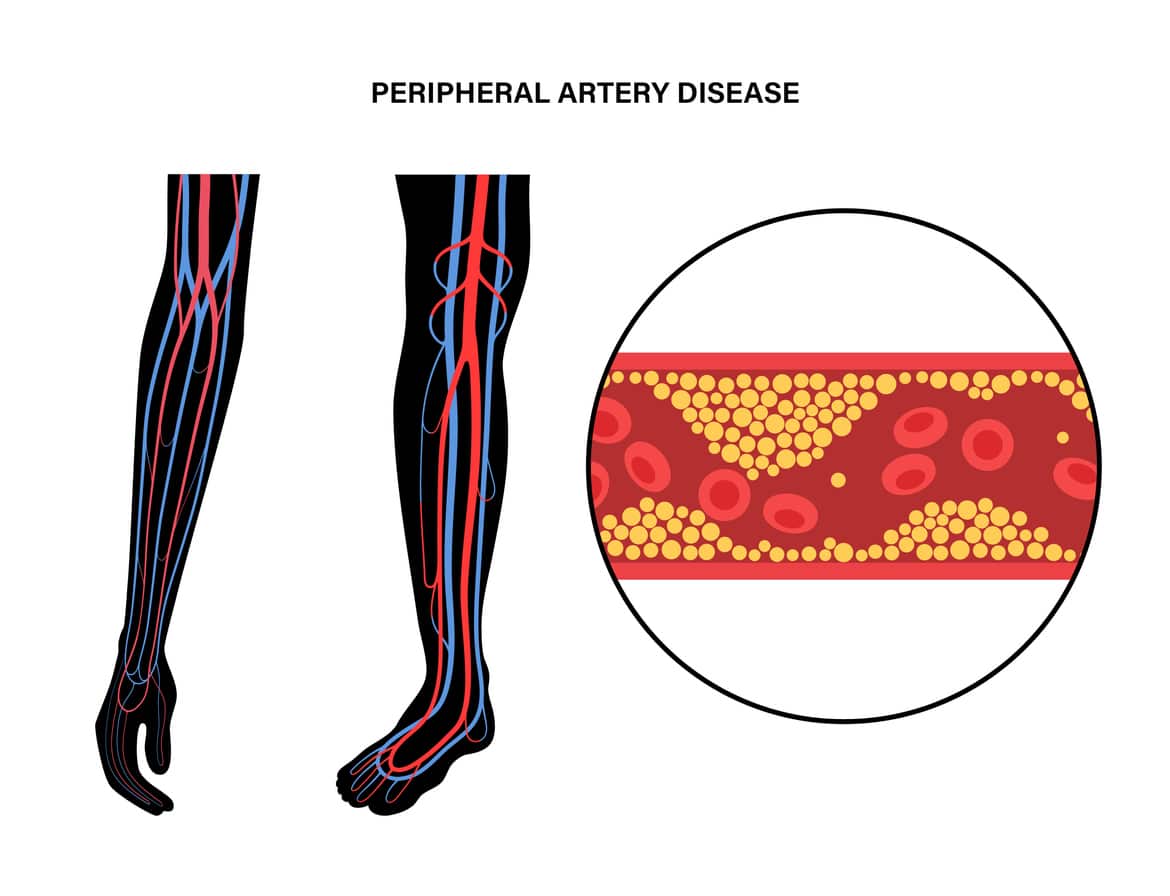
Peripheral artery disease is the result of plaque narrowing the arteries. It reduces blood flow to the extremities, leading to cold hands and feet.
Raynaud’s Syndrome
This disorder affects the small blood vessels in the fingers, toes, lips, nose, and ear lobes by causing them to spasm in cold weather and interrupt the blood flow.
Smoking Tobacco
Smoking cigarettes interferes with the circulatory system by narrowing blood vessels. This habit is especially problematic for the blood vessels in the feet. It is even associated with the development of Buerger’s disease. This disease causes the lining of the blood vessels to swell, restricting blood flow.
Stress and Anxiety
Stress and anxiety can trigger a tightening of the blood vessels, increased blood pressure, and inflammation in the body. All of these can have a detrimental effect on circulation.
Unhealthy Body Weight
Excess fat can lead to inflammation, impeding blood flow through the arteries. Being underweight can also lead to cold hands and feet, as the body attempts to conserve energy by diverting blood flow away from the extremities.
How to Help Cold Feet

In most cases, chilly feet are caused by temporary and medically insignificant conditions with obvious origins. On the other hand, chronically or unexplained cold feet or feet that are difficult to warm back up may indicate more serious conditions. As aforementioned, these include heart disease, diabetes, and hormonal imbalances. These should be addressed by a medical professional.
If your doctor has ruled out any serious underlying conditions, there are several ways to reduce the duration, intensity, and overall occurrences of frozen feet. Tips and tricks for keeping your feet comfortably warm include:
- Avoid spending time in cold environments, including frozen food aisles or directly in front of the air conditioner.
- Avoid stepping on cold surfaces, especially on bare feet.
- Get regular exercise.
- Maintain a healthy body weight.
- Manage stress.
- Use herbs and spices that improve circulation, such as:
- Black Pepper
- Cayenne
- Cinnamon
- Garlic
- Ginko Biloba
- Hawthorn Berries
- Turmeric
- Wear slippers in the house.
- Wear warm socks in cold weather.
Severe symptoms may require medication for relief. Some of the most commonly prescribed drugs for poor circulation include calcium channel blockers. These improve circulation by relaxing the smallest blood vessels. Additionally, alpha-blockers counteract the vasoconstricting hormone norepinephrine. For those experiencing circulation-related wounds, nitroglycerin skin ointment may also be offered to heal ulcers.
Although cold feet are a common condition, they can sometimes reveal hidden disorders. Consulting with a medical professional can help rule out and treat underlying conditions. Once any underlying conditions have been shown or ruled out, cardio exercises, a little extra time to relax, and a nice pair of warm socks certainly can’t hurt!
Warm Those Tootsies

Pros: Made with heavyweight wool while feeling soft and warm

Pros: Soft, comfortable, breathable, and wearable for cool days.

Pros: Available in 9 colors, made with a comfortable coral fleece upper and ultra-soft coral plush lining

Pros: Made with 100% Australian shearling, these slippers are comfortable and durable.
Read More:
Menopause Cold Flashes: Why They Happen and What to Do







