It’s no secret that heart disease remains the leading cause of death in the United States. According to the Centers for Disease Control and Prevention, it accounts for approximately one out of every four deaths. And while there are plenty of risk factors that you can control, such as diet, exercise, and smoking, there are other factors that are out of your hands, such as heredity, aging, and even gender.
The American Heart Association warns that although women are typically at lower risk for heart attacks than men, their chances of dying from a heart attack are actually greater, and the risk of death from heart disease increases once a woman reaches her menopausal years. One reason may be that the symptoms of heart disease in women aren’t always obvious.
“It can be tricky because women don’t always have the same symptoms that we typically relate to heart disease like chest pain,” explains Dr. Jorge Alvarez, a cardiologist in San Antonio, Texas. Things like increased fatigue, shortness of breath, or difficulty performing tasks that were once easy can all be early warning signs. “A lot of times, we shrug these things off as age, but it is important to mention them to your physician so an appropriate screening and evaluation can take place,” he adds.
Depending on symptoms, family history, and risk factors, that screening will usually begin with a traditional resting echocardiogram or “Echo” to get a clear picture of the heart’s structure. In some cases, this may be followed by a stress echocardiogram, or “stress test,” to determine how the heart responds to workload. Each of these tests has a specific function when it comes to the diagnosis of any cardiovascular issues.
Understanding the Echo
To understand how an Echo works, it helps to have a basic understanding of the intricate functions of the heart. Dr. Alvarez explains it by comparing the heart to a house. The heart muscle is the walls, which can be either thick or thin. The four valves of the heart are the doors, opening, and closing, to allow blood to flow in or out of the ventricles. The arteries serve as the plumbing, transporting the blood throughout the body, and the conduction system is the electricity that causes your heart to beat. All of these areas of the heart work together, and each one can affect or be affected by another.
Your doctor can identify structural cardiac issues like valve disorders or function issues like heart failure through an echocardiogram. The Echo can also identify many diseases that can affect the heart, either from the lungs or specific types of cancers. It can also be used to determine the cardiovascular effects of certain medications, such as chemotherapeutics.
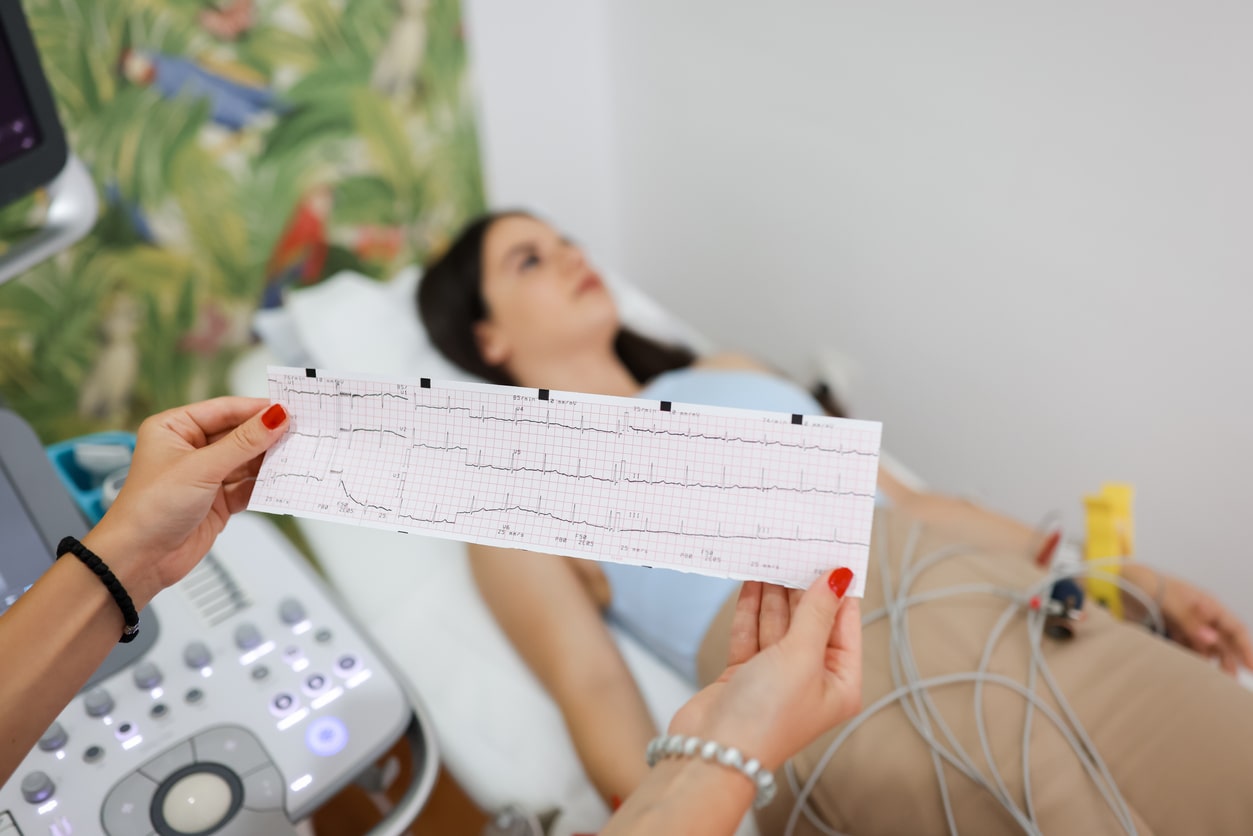
This common, painless procedure uses high-frequency sound waves to produce images of the chambers and valves of the heart. Performed by attaching adhesive electrodes to the chest that are hooked up to a monitor, it allows the doctor to observe how the heart is functioning. It can identify abnormalities in the size of the heart and any issues associated with the opening and closing of the valves. A wand with a gel-coated tip may be run across the chest to pick up the sound waves (Doppler signals) to determine both the speed and the direction of the blood moving through the heart.
“Echocardiograms are used to look for anatomical issues or to evaluate the heart function,” explains Dr. Alvarez. “It should always be the first test done, and then you progress from there.”
Don’t Stress the Stress Test.
If more information is needed, your doctor may request a cardiac “stress test.” Also called an exercise stress echocardiogram, the stress test is designed to monitor the heart’s response to physical activity.
Unlike the traditional echocardiogram, this procedure typically requires you to be in a fasted state and refrain from taking certain medications on the day of the test. It is usually performed on a treadmill that gradually increases in both speeds and inclines until a target heart rate is reached or you experience symptoms that require you to stop. A baseline echo is taken before the start of the stress test and again at the completion of the test for comparison.

“The stress test is done to evaluate for symptoms of possible coronary artery disease or to evaluate the functional capacity and ability to raise your heart rate or rhythm,” explains Dr. Alvarez, adding that there are alternatives to the treadmill test for those people who are unable to physically exercise. “There is a pharmacological stress test, where we use medication to induce the heart response to exercise while the patient is seated in a chair that gives us the results we need.”
When To Test
Unlike mammograms or colonoscopies, Alvarez says there is no recommended age for a screening stress test. Instead, a screening depends on your cardiovascular risk factors. Things like diabetes, hypertension, tobacco abuse, family history, and high cholesterol are all risk factors that should be considered. However, just because you don’t have high-risk factors doesn’t mean that you should ignore any symptoms. As Dr. Alverez mentioned earlier, this is especially true for women.
“The cornerstone symptom would be chest pain, but, as I said earlier, that isn’t always the case for women,” he says. “A simple change in functional capacity can often be the earliest symptom.”

It is never too late to develop heart-healthy habits. Control what you can in terms of your diet, activity level, and lifestyle, and keep your doctor informed of any risk factors. Consult your doctor if you begin to notice things like extreme fatigue or shortness of breath while going about your daily activities or if you experience a decrease in your exercise tolerance. Being in touch with your body and advocating for yourself when you suspect something isn’t “right” may just save your life.
This article is for informational purposes only and is not intended to diagnose or treat any medical conditions. Consult with your doctor if you think you have any medical issues or if you’re considering adding any supplements or medications to your daily routine.
Read Next:
Recognize and Prevent Heart Disease